What you need to know about bivalent boosters for COVID-19
The SARS-CoV-2 omicron variant has frustrated citizens and experts alike with its ability to evade immunity from vaccines and prior infections.
Fortunately, the FDA has authorized a new bivalent booster shot, also known as an "updated booster," targeting both the original strain of SARS-CoV-2 and omicron subvariants BA.4 and BA.5, which should be available in the U.S. this fall.
Bloomberg School experts Andrew Pekosz, a professor in Molecular Microbiology and Immunology; Anna Durbin, a professor in International Health; and William Moss, a professor in Epidemiology and the executive director of the International Vaccine Access Center, recently shared their insights into bivalent vaccines and their potential to help curb COVID-19 transmission.
What are bivalent vaccines?
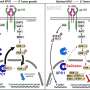
Willam Moss: The current COVID-19 mRNA vaccines contain the genetic recipe for the spike protein of the original strain isolated and sequenced from Wuhan, China.
Anna Durbin: The bivalent vaccine will contain the genetic recipes for two versions of the spike protein: the original strain, plus spike proteins from the omicron subvariants BA.4 and BA.5.
When will they be available?
AD: After FDA authorization, the vaccines will need approval from the Advisory Committee on Immunization Practices. The approval process for the first mRNA COVID vaccines moved very quickly, taking only a couple of weeks. Once this process is complete, the new vaccines should be available shortly afterward.
Who will be eligible to receive this booster?
WM: It is expected that the Pfizer-BioNTech vaccine will be authorized for use as a booster dose in individuals 12 years and older, and the Moderna bivalent vaccine as a booster dose in individuals 18 years and older. However, vaccine supplies may be limited in the months after authorization, and high-risk groups such as older adults may be prioritized initially.
Can bivalent vaccines be used as an initial course of vaccination?
AD: Theoretically yes, but you would need two doses if it is the initial course of vaccination.
Andrew Pekosz: At this time, however, the bivalent vaccine is considered only a booster, not a means of primary vaccination. For the foreseeable future, any adult starting a COVID-19 vaccination schedule will receive the original COVID-19 vaccine for their initial shot.
Do you have to wait 90 days after having COVID to get a bivalent vaccine?
AD: No specific timeline has been established for the bivalent vaccine, but in general, it is better to wait a while—most experts recommend at least a month—after getting COVID to get vaccinated.
AP: I hope this question will be addressed in the FDA/CDC recommendations for the bivalent booster. Ideally, they will specify how long after a booster dose or infection individuals should wait before receiving a bivalent booster shot. Regardless, for optimal, long-term responses, boosters should be spaced out.
WM: This is an important question for those who got or are considering a booster dose now. High-risk individuals would benefit from a booster dose now and will still be eligible to receive the bivalent vaccine this fall depending on the FDA and ACIP recommendations on the minimum interval between booster doses.
How long do you have to wait after receiving your last booster (specifically, either the third or fourth dose of the original mRNA COVID-19 vaccine) to get a bivalent vaccine?
AD: A firm answer awaits FDA/CDC guidance, but experts suggest waiting at least one to two months if you are not at high risk of serious illness.
AP: Agreed. I might even suggest six months as an ideal interval to ensure the best immune response to the booster.
Does immunity still take two weeks to develop after this shot?
AD: Antibody titers start to rise within days after getting the shot, but it will probably take a couple of weeks to get the highest amount of antibodies.
Will bivalent vaccines eventually completely replace the original COVID vaccines?
AP: The aim of the COVID-19 vaccine campaign is to generate the strongest and broadest immunity against all variants, including pre-omicron variants.
Data suggests that this goal can be accomplished with initial two-dose vaccinations focused on the original COVID-19 strain and then a bivalent booster. Any changes to this strategy would require clinical testing, but that's nearly impossible—there just aren't enough adults left who haven't been infected or vaccinated to perform a valid test.
WM: Another unknown is whether the BA.4/BA.5 omicron subvariants will continue to be the dominant viruses or whether we will see novel and different variants for which modified vaccines will need to be developed, much as we update influenza vaccines each year.
We know the bivalent vaccine will help prevent severe disease, but will it prevent people from getting infected with COVID at all?
AP: The most likely scenario is strong protection from severe disease and hospitalization, with variable protection from infection. It may prevent infection for a time, but we don't know for how long.
AD: It is very hard to prevent infection entirely with respiratory viruses. You can get re-infected after a natural respiratory viral infection, so totally preventing COVID infection for long periods of time is not likely to be accomplished with a vaccine.
WM: Boosters with nasal vaccines, which are being developed, may do a better job at preventing infection by inducing mucosal immunity in the upper airway.
Who will benefit most from bivalent vaccines?
AD: Those who are most likely to get more severe disease: the elderly, immunocompromised, and those with comorbid conditions like diabetes, kidney disease, and underlying lung disease.
AP: I agree, but the recommendation will be for every adult to be boosted, which needs to happen to help reduce spread of the virus in the population.