New research identifies potential treatment to manage effects of periodontitis
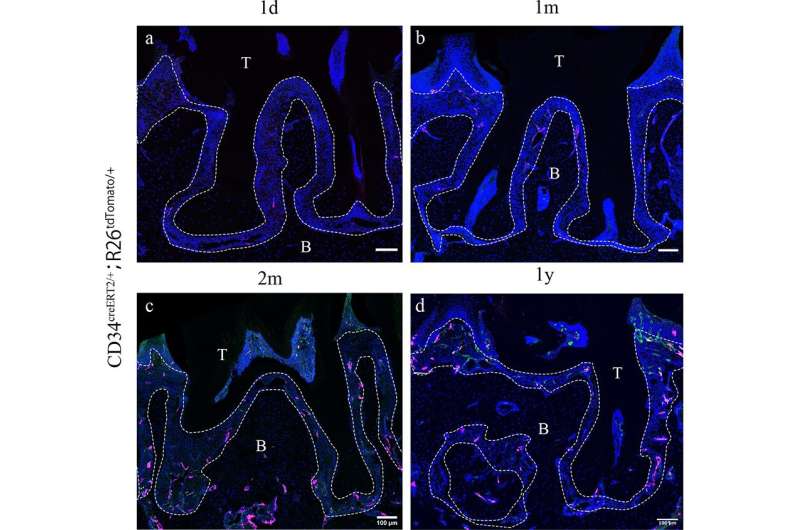
A new study from King's College London has identified the potential of a cell type known as a telocyte to be used to manage the effects of periodontitis.
Periodontitis is a severe gum infection that can lead to tooth loss and other serious health complications. It is an incurable and continuous degenerative disease and, without treatment, can destroy the bone that supports teeth.
Macrophages are important cells of the immune system that are formed in response to an infection or accumulating damaged or dead cells. Macrophages that encourage inflammation are called M1 macrophages, whereas those that decrease inflammation and encourage tissue repair are called M2 macrophages. Macrophages are known to infiltrate infected periodontal tissue and are a significant part of the inflammatory process.
The balance between M1 & M2 macrophages is important for regulating immune responses with tissue repair processes. The study, from the Sharpe lab in the Centre for Craniofacial and Regenerative Biology, identified the role of an unusual cell type, the telocyte, in regulating the M1-M2 macrophage balance in periodontitis and showed the natural ability to shift M1 to M2. This may provide a route for therapeutic interventions to limit inflammation and bone loss in periodontitis.
"I hope this study can not only lead to a greater understanding of periodontal disease but also provide an impetus for others to study the potential roles played by telocytes in other tissues. My special thanks must go to all involved in this COVID-interrupted research who stepped in to fill the gaps," says Professor Paul Sharpe, corresponding author.
Understanding the regulation of the inflammatory response is critical to understanding and treating periodontitis. The build up of plaque on the tooth surface invades the periodontium tissue and releases a bacterial toxin lipopolysaccharide, which in turn causes the polarization of the pro-inflammatory M1 macrophages. By analyzing individual cells in the periodontal tissue, the study showed that telocytes are activated in disease to grow and release a factor (HGF) that shifts macrophages from an M1 to an M2 state.
The research demonstrates for the first time that telocytes increase in number in periodontitis and communicate with immune cells to positively impact the effects of periodontitis via HGF. The resulting transition of macrophages provides a possible strategy for treating periodontitis. The function of telocytes may also present in other inflammatory disease where telocytes exist such as arthritis and cancer research.
The research was published in eLife.
More information: Jing Zhao et al, Telocytes regulate macrophages in periodontal disease, eLife (2022). DOI: 10.7554/eLife.72128