This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
trusted source
proofread
How tumors transform blood vessels
Increasingly dense cell clusters in growing tumors convert blood vessels into fiber-filled channels. This makes immune cells less effective, as findings by researchers from ETH Zurich and the University of Strasbourg suggest. Their research is published in Matrix Biology.
It was almost ten years ago that researchers first observed that tumors occurring in different cancers—including colorectal cancer, breast cancer and melanoma—exhibit channels leading from the surface to the inside of the cell cluster. But how these channels form, and what functions they perform, long remained a mystery.
Elaborate and detailed experiments
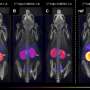
Through a series of elaborate and detailed experiments, the research groups led by Viola Vogel, Professor of Applied Mechanobiology at ETH Zurich, and Gertraud Orend from the University of Strasbourg have found possible answers to these questions. There is a great deal of evidence to suggest that these channels, which the researchers have dubbed tumor tracks, were once blood vessels.
These blood vessels start out by supplying the fast-growing cell clusters with glucose and oxygen. But then the vessels undergo a process that strips them of their original function of transporting blood: the vessel walls change and the vessel cavity gradually fills up.
When fibers control the behavior of immune cells
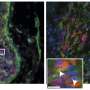
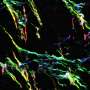
This filler material consists mainly of cells and newly formed protein fibers, which make up what is known as the extracellular matrix. Collagen fibers are found here, as are fibronectin fibers. The latter play a role in growth processes that take place mainly during embryonic development or wound healing. In their article, the researchers show that the fibers within the tumor tracks are capable of trapping immune cells.
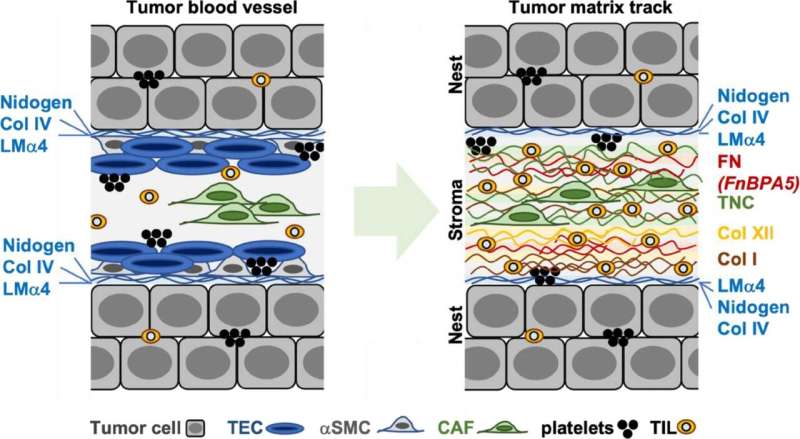
While this happens, the immune cells stretch out along the channels and stick to the loose fibronectin fibers. "In this elongated form, the immune cells switch from fighting diseases to supporting healing processes," Vogel says. Instead of attacking the tumor cells, they excrete molecules that stimulate growth, thus helping the cancer cells to multiply.
The previously unknown role of tissue tension
It becomes clear that the tension of extracellular matrix fibers plays a key and previously unknown role in tumor development: in healthy tissue, the fibronectin fibers are stretched extremely taut; only in tumor tissue are they slack. In this looser, more relaxed form, surrounded by transformed blood vessel walls, the fibronectin fibers evidently create a recess in which cancer cells can grow undisturbed.
Vogel says that the main focus of cancer research has been on the cells: "The extracellular matrix was frequently overlooked." That's why the crosstalk between cells and their environment still remains a mystery. "But if you want to understand what a spider does, you also have to look at its web," she says.
Investigating tissue samples from patients
Vogel therefore also sees the new findings as a reason to expand her research focus and gain a better understanding of the bigger picture. "The better we understand how the microenvironment steers how tumor cells multiply, the likelier it is that we'll find a way of preventing them from doing so," she says.
Vogel does, however, cautions to translate the implications of the results to humans because they are based on experiments on mice with breast cancer. It remains to be seen whether or not these results can be applied directly to cancers in humans. But there are indeed several parallels, as Orend's group external recently demonstrated.
Meanwhile, Vogel's research group has started collaborating with the Kantonsspital Baden on a follow-up project: one of Vogel's doctoral students is investigating if tissue samples taken from breast cancer patients also contain traces of converted blood vessels. "We're curious to discover where we'll find similarities and where we'll see differences," Vogel says.
More information: Charlotte M. Fonta et al, Infiltrating CD8+ T cells and M2 macrophages are retained in tumor matrix tracks enriched in low tension fibronectin fibers, Matrix Biology (2023). DOI: 10.1016/j.matbio.2023.01.002
Devadarssen Murdamoothoo et al, Tenascin‐C immobilizes infiltrating T lymphocytes through CXCL12 promoting breast cancer progression, EMBO Molecular Medicine (2021). DOI: 10.15252/emmm.202013270