This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
trusted source
proofread
Biological factors modulate eating disorder risk in early adolescents
Genetic and neurobiological factors shape the development of eating disorders much earlier than previously thought, with evidence emerging in children as young as nine years old, Yale-led research reveals. The findings, researchers say, highlight the need for early screening and intervention.
The results were published July 27 in Nature Mental Health.
Eating disorders, such as anorexia nervosa, bulimia nervosa, and binge-eating disorder, often emerge during adolescence. And while previous research has shown these disorders have genetic components (heritability is between 40 and 70%) as well as neurological aspects, the relationships between these factors aren't fully understood.
"We know that, like many other mental health conditions, the rates of eating disorders increase in adolescence, and that could be related to both changes in how the brain develops during this period as well as genetic factors," said lead author Margaret Westwater, a laboratory associate and former postdoctoral fellow at Yale School of Medicine.
"But we don't fully understand the mechanisms by which genetic risk or brain structure can influence your risk for eating disorders, particularly during the critical developmental period of adolescence."
Westwater is part of the lab of Yale's Dustin Scheinost, an associate professor of radiology and biomedical imaging and co-author of the study.
To better understand what biological factors might be at play when it comes to the development of eating disorders, the research team used data from the National Institutes of Health's Adolescent Brain and Cognitive Development Study, the largest long-term study of brain development and child health in the United States. They assessed genetic risk, brain structure, and eating disorder symptoms in more than 4,900 adolescents aged 9 to 11.
They found that genetic risk for high body mass index (BMI) was associated with eating disorder symptoms, but not symptoms of anxiety, depression, or obsessive-compulsive disorder.
"That was a little surprising because there's evidence in adults that genetic risk for high BMI is associated with depression, but that's not what we found in this younger group," said Westwater.
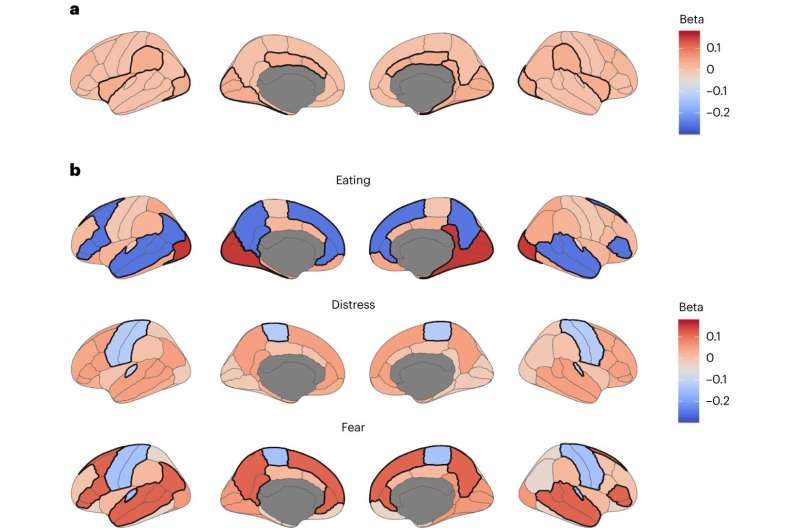
The researchers also found that the genetic risks for BMI and for anorexia were correlated with different brain structures. Specifically, high BMI risk is associated with greater cortical thickness in certain brain regions and widespread reductions in brain surface area while anorexia risks are associated with reduced volume of the caudate. The caudate, which lies deeper in the brain, is associated with motor control and higher order cognition like learning and decision making.
"We know from past research that there is likely something going on with the caudate in terms of the pathogenesis of anorexia nervosa," said Westwater. "But here we're finding a link in children who have higher genetic risk for anorexia, but do not have anorexia itself. It could suggest that reduced caudate volume might be a risk factor for transition to this illness."
Additionally, the research team found that eating disorder symptoms were associated with greater thickness of the visual brain network and reduced thickness across a brain network that's active when someone is in a more cognitively restful state and not focused on their external environment.
"Patients with eating disorders struggle with intrusive thoughts about body image or food," Westwater said. "So it might be that some underlying difference in the structure of these brain networks is contributing to those symptoms."
One of the big takeaways from the findings, she added, is that biological factors are shaping eating disorder development at a very early age.
"While we've recognized for a long time that eating disorders emerge during adolescence, this is one of the first pieces of evidence to suggest that there are genetic and neurobiological mechanisms modulating someone's risk for these conditions by the age of 10, which is much earlier than most people associate with eating disorders," said Westwater. "It underscores the need for screening in schools and primary care settings as well as early intervention to save folks from years of suffering."
More information: Margaret L. Westwater et al, Assessing a multivariate model of brain-mediated genetic influences on disordered eating in the ABCD cohort, Nature Mental Health (2023). DOI: 10.1038/s44220-023-00101-4



















