Inhibiting Hedgehog signaling pathway may improve pancreatic cancer treatment
Combining a new targeted therapy with standard chemotherapy may help defeat pancreatic cancer, according to results presented at the American Association for Cancer Research's Pancreatic Cancer: Progress and Challenges conference, held here June 18-21.
"We believe that GDC-0449 has the potential to change the approach to treating pancreatic cancer," said Edward J. Kim, M.D., Ph.D., a medical oncologist at the University of Michigan Comprehensive Cancer Center in Ann Arbor, Mich.
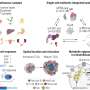
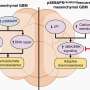
GDC-0449 targets the Hedgehog signaling pathway. This pathway is normally silent in the adult pancreas but it is switched on in patients with pancreatic cancer and contributes to the desmoplastic stroma that is characteristic of this disease.
"This dense stroma is believed to contribute to resistance to chemotherapy by presenting a physical barrier to chemotherapy delivery," Kim explained.
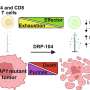
In addition, Hedgehog levels are increased in pancreatic cancer stem cells. Cancer stem cells are a subset of cancer cells present in a tumor that are believed not only to drive tumor growth by generating bulk tumor cells, but to also be particularly resistant to standard therapies like chemotherapy and radiation.
"Even if a therapy succeeds in obtaining a response, cancer stem cells may persist and contribute to resistance and progression of disease," Kim said. "Having found that pancreatic cancer stem cells have higher Hedgehog levels than bulk cancer cells, we were interested in determining whether targeting the Hedgehog signaling pathway and, therefore, the cancer stem cells might lead to improved outcomes in pancreatic cancer."
GDC-0449 targets the Smoothened (SMO) protein in the Hedgehog signaling pathway. It was approved for use in basal cell carcinoma and is marketed as vismodegib. Kim and his colleagues felt that treating patients with pancreatic cancer first with GDC-0449 and then with the standard chemotherapeutic drug gemcitabine might disrupt the desmoplastic stroma and improve the efficacy of the chemotherapy.
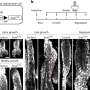
They evaluated this strategy in treatment-naive patients with advanced pancreatic cancer. Patients underwent needle biopsies of the cancer before and after taking GDC-0449 for three weeks to study the effects of GDC-0449 on the Hedgehog pathway signals, tumor stroma and pancreatic cancer stem cells. Gemcitabine was added to GDC-0449 following the second biopsy.
Five patients achieved partial response, and another four patients had stable disease, yielding a 50 percent progression-free survival rate at three months.
"New ways to treat pancreatic cancer are needed to improve response to therapy and ultimately patient outcomes," Kim said, adding that he hopes data from the biopsy specimens will help identify predictive markers to determine who would benefit from this combination treatment.
More information:
Abstract
Cancer stem cells (CSC) and inhibition of hedgehog (Hh) pathway signaling in advanced pancreatic cancer: GDC-0449 in combination with gemcitabine (Gem). Edward J. Kim1, Gazala N. Khan1, Kent Griffith1, Joel Greenson1, Naoko Takebe2, Mark Zalupski1, Diane Simeone1. 1University of Michigan, Ann Arbor, 2NIH, Rockville, MD.
Background: Pancreatic CSCs are a highly resistant subpopulation within a tumor that possess stem cell properties such as self-renewal and exhibit greater tumorigenicity and metastatic potential. These features are associated with reactivation of developmental pathways including the Hh signaling pathway. We previously reported that CD44+/CD24+/ESA+ pancreatic CSCs express significantly elevated levels of Sonic Hh (Cancer Res, 2007). GDC-0449, a Smoothened antagonist, is an orally delivered small molecule inhibitor of the Hh pathway that has been evaluated in Phase 1 studies. We report here preliminary results of a clinical trial in patients with metastatic pancreatic cancer investigating sequential delivery of GDC-0449 and Gem providing a rationally designed, novel multi-targeted therapy. This trial importantly includes prospective evaluation of Hh pathway inhibition in pancreatic cancer by incorporating paired core biopsies of tumor before and after treatment with GDC-0449.
Materials and Methods: Patients with previously untreated, metastatic pancreatic cancer were eligible. GDC-0449 was initiated as daily monotherapy for a 4-week cycle followed by the combination of daily GDC-0449 with intravenous Gem days 1, 8 and 15 for each subsequent cycle. Two sets of 3 core biopsies were performed on each patient; one set prior to start of therapy and a second set 3 weeks after beginning GDC-0449. A primary trial objective was to evaluate effects of GDC-0449 on pancreatic CSCs. Tumor biopsies were processed immediately after biopsy and allocated for correlative experiments. Fresh tissue was analyzed for CD44, CD24, and ESA expression by flow cytometry. Formalin-fixed tumor samples were evaluated for Ki67 by immunohistochemistry (IHC) and a proliferative index was calculated. Pre-treatment Sonic Hh expression was also analyzed by IHC and assigned an H-Score based on review by a pancreatic pathologist. Clinical outcome parameters were measured, including progression free survival (PFS) at 3 months and response rate, and overall survival.
Results: Twenty of a planned 25 patients have been accrued and undergone paired biopsies with 18 of 20 patients assessable for response after 3 cycles of therapy. Although a subset of patients had evidence of disease progression on GDC-0449 monotherapy per RECIST criteria, continuation of GDC-0449 with addition of Gem resulted in significant response in several patients. RECIST-defined confirmed partial response was achieved in 5 patients (28%) with 4 additional patients having stable disease, yielding a 50% PFS rate at 3 months. Three patients have received treatment for ≥12 cycles. The percentage of pancreatic CSCs decreased in 56% of patients, and of these patients, the mean relative decrease was 60% ±22% (range, 16-87%). Proliferative index decreased in 54% of the patients (range, -11% to +28%). Sonic Hh expression was more highly expressed in patients that achieved a partial response or stable disease as compared to those with progression (mean H-score 285 vs 168, p = 0.016). Ongoing analysis of the effect of GDC-0449 on Hh pathway target genes is being conducted.
Conclusion: Sequential delivery of GDC-0449 as monotherapy followed by combination with Gem is effective in providing clinical benefit to a subset of patients with metastatic pancreatic cancer. Of the biological correlates evaluated, pre-treatment Sonic Hh expression level is the best predictor of benefit with this regimen. Ongoing correlative studies are underway to further refine the best predictor of who will benefit from this combination therapy.