One protein, two personalities: Study identifies new mechanism of cancer spread
Cancer involves a breakdown of normal cell behavior. Cell reproduction and movement go haywire, causing tumors to grow and spread through the body.
A new finding by University of Pennsylvania scientists has identified key steps that trigger this disintegration of cellular regulation. Their discovery—that a protein called Exo70 has a split personality, with one form keeping cells under tight control and another contributing to the ability of tumors to invade distant parts of the body—points to new possibilities for diagnosing cancer spread.
The research, published in the journal Developmental Cell, was conducted by a team comprised of researchers from the School of Arts and Sciences' Department of Biology; the Perelman School of Medicine's pathobiology and laboratory medicine, medicine and genetics departments, and China's Hangzhou Normal University School of Medicine.
"It turns out that one form of Exo70 is important in maintaining 'law and order' in cells, keeping them structured and organized in tissues" said senior author Wei Guo, an associate professor of biology, "while the other form promotes cell movement."
This was not the first time that Guo's group had focused on Exo70, which plays a role in the process known as exocytosis, by which cells transport proteins and other molecules such as hormones and neurotransmitters to the membrane and release them. In previous work, combining biochemistry, ultrastructure cell imaging and mathematical modeling, they showed that Exo70 and a host of other proteins, collectively known as the exocyst, are involved in cell migration, and that Exo70 itself is critical for cell membranes to initiate movement by bending the cell's plasma membrane.
But it turns out that the Exo70 they were studying was only one of five forms present in cells. In the current work, they found that one of these forms was associated with epithelial cells, which line the body's organs and cavities. They called this form Exo70E. The form they had studied in previous work was associated with mesenchymal cells, or cells that are highly motile. They called this form Exo70M.
The fact that these forms associated with epithelial and mesenchymal cells, respectively, caused the researchers to think about a process called the epithelial-mesenchymal transition, or EMT. In it, epithelial cells, which are normally tightly packed together and structured, acquire the ability to migrate. EMT is a normal part of cell biology that occurs in processes such as neural tube formation and wound healing, but also occurs at the beginning of cancer metastasis.
To see what role Exo70 might be playing in EMT, the researchers studied a laboratory cell line in which they could induce EMT. As the transition occurred, they observed that levels of Exo70E declined while Exo70M rose. They found that a protein called epithelial splicing regulatory protein 1, or ESRP1, appeared to play a role in switching between forms, promoting the Exo70E form and preventing EMT from occurring. ERSP1 itself has been shown by Perelman School of Medicine researchers, including Associate Professor of Medicine Russ Carstens, to be a major regulator in EMT.
Experimenting further to investigate how the two forms of Exo70 affected cell behavior, the team found that adding Exo70E to mesenchymal cells caused them to look more like epithelial cells, retaining structure and inhibiting movement. When they inhibited all forms of Exo70 in a line of breast cancer cells, the tumor cells lost their ability to migrate, a necessary part of tumor invasion. Adding back Exo70M, however, allowed these cells to regain their ability to migrate and invade, while Exo70E did not.
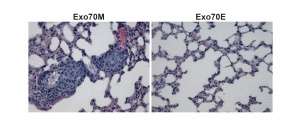
These results were upheld in experiments in mice. The researchers inoculated the mice with breast cancer cells that had been genetically engineered to express either Exo70E or Exo70M. Normally, the cancerous cells would spread all around the body and indeed, this is what the researchers saw in the mice exposed to the cells with the Exo70M form. But there was no evidence of such metastasis in mice given cells expressing only Exo70E.
"In this case, Exo70E was behaving almost like a tumor suppressor," Guo said.
Finally, to see if their findings would be clinically relevant in humans, the researchers looked for the different forms of Exo70 in tissue from human breast cancer patients.
"We found that patients who had a high E-to-M form ratio had cancers that were less likely to have spread," Guo said. "Patients who had cancers that spread to the lymph nodes had more of the M form."
Such a finding offers a potential biomarker for clinicians to judge the progression of cancers, or the likelihood of a particular case of cancer to spread.
More information: dx.doi.org/10.1016/j.devcel.2013.10.020