Team finds potential clue associated with aggressive prostate cancer
Prostate cancer is one of the most common forms of cancer in men and the leading cause of cancer deaths in white, African-American and Hispanic men, according to the Centers for Disease Control. Current treatment of prostate cancer targets androgens, hormones which promote the growth and spread of cancer cells. However, it remains unclear why, despite treatment, some prostate cancers progress and may become fatal. Researchers at Robert Wood Johnson Medical School, part of Rutgers, The State University of New Jersey, who are studying the underlying mechanisms that cause invasive tumor growth have identified a key transcription factor, a protein which regulates the flow of information from DNA, that is over-produced in treatment-resistant prostate cancer, as well as the two protein kinases that trigger the process.
This finding, published and highlighted on the cover of the July issue of Molecular Cancer Research, a journal of the American Association for Cancer Research (AACR) could be utilized to develop treatments for prostate cancer that is resistant to current therapies.
The research team, led by Joseph Fondell, PhD, associate professor of pharmacology, found that in clinically localized human prostate cancer—cancer that is confined to the prostate and pelvic area—the key transcription factor termed MED1 is overexpressed, meaning that significantly more MED1 is produced than is typical. According to Fondell, the finding potentially could be used as a biomarker in cancer screenings, indicating to oncologists that the prostate cancer has become aggressive. "As MED1 is a known co-activator of androgen receptors, the overexpression of MED1 is thought to facilitate alternative gene expression patterns that drive treatment-resistant cancer cell growth in the prostate," Fondell said.
"Our study showed for the first time that MED1 expression is elevated in malignant cells of a statistically significant number of patients with clinical prostate cancer and that this overexpression correlates with an increase in cancer cell growth and invasiveness," said Feng Jin, PhD, a former graduate student in Fondell's lab and first author on the study. "In addition to accelerated tumor growth, our study showed that overexpression of MED1 may also be involved with inflammation of the prostate."
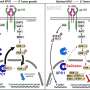
Further study of the process using mouse models that mimic human prostate cancer, showed that two protein kinases, ERK and PI3K/AKT, were overactive and responsible for MED1 overproduction, ultimately accelerating the progression and spread of prostate cancer.
"Whereas the current treatment approach for prostate cancer is to prohibit androgen production and signaling, our findings indicate that MED1 could represent a novel target for new therapies that stop the process at the molecular level, before prostate cancer can progress to an advanced stage," added Fondell, who also is a member of Rutgers Cancer Institute of New Jersey.
More information: mcr.aacrjournals.org/content/11/7/736.abstract