Will stem cell therapy help cure spinal cord injury?
A systematic survey of the scientific literature shows that stem cell therapy can have a statistically significant impact on animal models of spinal cord injury, and points the way for future studies.
Spinal cord injuries are mostly caused by trauma, often incurred in road traffic or sporting incidents, often with devastating and irreversible consequences, and unfortunately having a relatively high prevalence (250,000 patients in the USA; 80% of cases are male). High-profile campaigners like the late actor Christopher Reeve, himself a victim of sports-related spinal cord injury, have placed high hopes in stem cell transplantation. But how likely is it to work?
This question is addressed in a paper published 17th December in the open access journal PLOS Biology by Ana Antonic, David Howells and colleagues from the Florey Institute and the University of Melbourne, Australia, and Malcolm MacLeod and colleagues from the University of Edinburgh, UK.
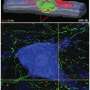
Stem cell therapy aims to use special regenerative cells (stem cells) to repopulate areas of damage that result from spinal cord injuries, with the hope of improving the ability to move ("motor outcomes") and to feel ("sensory outcomes") beyond the site of the injury. Many studies have been performed that involve animal models of spinal cord injury (mostly rats and mice), but these are limited in scale by financial, practical and ethical considerations. These limitations hamper each individual study's statistical power to detect the true effects of the stem cell implantation.
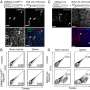
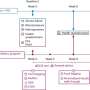
This new study gets round this problem by conducting a "meta-analysis" – a sophisticated and systematic cumulative statistical reappraisal of many previous laboratory experiments. In this case the authors assessed 156 published studies that examined the effects of stem cell treatment for experimental spinal injury in a total of about 6000 animals.
Overall, they found that stem cell treatment results in an average improvement of about 25% over the post-injury performance in both sensory and motor outcomes, though the results can vary widely between animals. For sensory outcomes the degree of improvement tended to increase with the number of cells introduced – scientists are often reassured by this sort of "dose response", as it suggests a real underlying biologically plausible effect.
The authors went on to use their analysis to explore the effects of bias (whether the experimenters knew which animals were treated and which untreated), the way that the stem cells were cultured, the way that the spinal injury was generated, and the way that outcomes were measured. In each case, important lessons were learned that should help inform and refine the design of future animal studies. The meta-analysis also revealed some surprises that should provoke further investigation – there was little evidence of any beneficial sensory effects in female animals, for example, and it didn't seem to matter whether immunosuppressive drugs were administered or not.
The authors conclude: "Extensive recent preclinical literature suggests that stem cell-based therapies may offer promise; however the impact of compromised internal validity and publication bias means that efficacy is likely to be somewhat lower than reported here."
More information: Antonic A, Sena ES, Lees JS, Wills TE, Skeers P, et al. (2013) Stem Cell Transplantation in Traumatic Spinal Cord Injury: A Systematic Review and Meta-Analysis of Animal Studies. PLoS Biol 11(12): e1001738. DOI: 10.1371/journal.pbio.1001738