Same cell death pathway involved in three forms of blindness
Gene therapies developed by University of Pennsylvania School of Veterinary Medicine researchers have worked to correct different forms of blindness. While effective, the downside to these approaches to vision rescue is that each disease requires its own form of gene therapy to correct the particular genetic mutation involved, a time consuming and complex process.
Hoping to develop a treatment that works more broadly across diseases, a Penn Vet team used canine disease models to closely examine how retinal gene activity varied during the progression of three different forms of inherited vision disease. Their results turned up an unexpected commonality: Early on in each of the diseases, genes involved in the same specific pathway of cell death appeared to be activated. These findings point to possible interventions that could curb vision loss across a variety of inherited retinal diseases.
The work, published in PLOS ONE, was conducted by Sem Genini, a senior research investigator; William A. Beltran, assistant professor of ophthalmology; and Gustavo D. Aguirre, professor of medical genetics and ophthalmology, all of Penn Vet's Department of Clinical Studies, Philadelphia.
The team examined three forms of retinal degenerative diseases, rod cone dysplasia 1 being the most severe, or earliest onset, followed by X-linked progressive retinal atrophy 2 and then early retinal degeneration. All of these diseases involve the death of photoreceptor cells and each is caused by a distinct genetic mutation. But what scientists did not know is how the mutations trigger a molecular signaling pathway that leads to the death of photoreceptor cells.
"What we have in mind is to be able to address multiple forms of disease with one treatment," Beltran said. "We wanted to get a better understanding of whether there are any common cell death or cell survival pathways that could be targeted in some of these diseases."
The researchers looked at the activity of 112 genes in diseased retinas and compared it to gene activity in normal retinas. They assessed gene activity at time points known to correspond with key phases of disease: the "induction phase," the time before the peak level of photoreceptor cell death; the "execution phase," when the highest rates of photoreceptor cell death occur; and the "chronic phase," during which photoreceptor cell death continues at somewhat reduced levels.
During the execution and chronic phases of disease, the researchers identified a number of genes involved in programmed cell death, or apoptosis, that had noticeably different patterns of expression between the diseased and normal dogs.
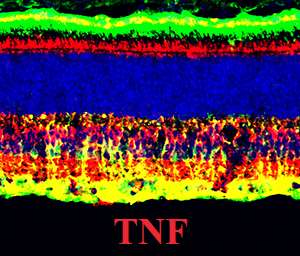
Of note, several proteins involved in the tumor necrosis factor, or TNF, pathway increased in activity during the induction and execution phases. This pathway is implicated in many diseases, from diabetes to cancer to rheumatoid arthritis.
"This is quite a new result," Genini said. "It was not expected to have the TNF pathway upregulated."
"We assumed," Aguirre said, "the diseases would be different from one another and that cells would commit suicide by their own specific pathway and that perhaps quite late they would have a common final pathway. But what this shows is that there is an early trigger that is quite similar among all three diseases."
An additional surprise was that the differentially expressed proteins were present not only in photoreceptor cells but also in other cells in the retina, including horizontal and Müller cells.
"We were focusing on what would happen with the photoreceptor cells, the cells that we knew were dying," Beltran said. "But what our results are telling us is that, sure, they are dying, but there is something else happening with the cells that they talk to."
Pharmaceutical companies have already developed TNF-inhibitors to treat diseases like rheumatoid arthritis. Genini, Beltran and Aguirre say their results suggest that these drugs or similar ones might have a role to play in the retinal diseases they investigated and perhaps in others that their team is currently studying.
"On its own," Beltran said, "a TNF-inhibitor might not be a cure, but it could be used complementary to gene therapy, either by slowing the course of degeneration before the corrective gene therapy is delivered or in combination with the corrective gene therapy."
More information: www.plosone.org/article/info%3Adoi%2F10.1371%2Fjournal.pone.0085408