New possible target to combat muscle wasting
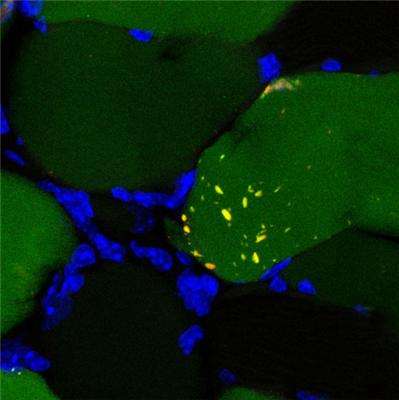
The pathological atrophy of skeletal muscle is a serious biomedical problem for which no effective treatment is currently available. The most affected populations are the elderly diagnosed with sarcopenia and patients with cancer, AIDS, and other infectious diseases that develop cachexia.
A study by scientists at the Institute for Research in Biomedicine (IRB), headed by Antonio Zorzano, also full professor of the University of Barcelona, reveals a potential therapeutic target to tackle muscle wasting in these risk populations.
In the study published today in the Journal of Clinical Investigation (JCI), one of the journals with highest impact in experimental medicine, the researchers associate the activity of the DOR protein with muscle atrophy and point to DOR as a plausible target against which to develop a drug to prevent muscle deterioration in certain diseases.
DOR (Diabetes- and Obesity-regulated gene), also known as TP53INP2, is a protein involved in autophagy, a quality control process that ensures cells stay healthy. The researchers have found that increased DOR expression in the muscle of diabetic mice leads to enhanced autophagy, which in turn favours the loss of muscle mass in these animals.
The advantage of developing a DOR inhibitor is that autophagy, a process necessary to keep cells healthy, would not be completely blocked in the absence of this protein. DOR is not essential for autophagy, but acts more as an accelerator. Thus, the inhibition of DOR would only partially reduce autophagy as other molecules involved would exert their activity normally, thus maintaining the levels of autophagy in a beneficial range for cells.
"If we could treat patients with sarcopenia and cachexia, or people at risk of these conditions, using a drug to inhibitor DOR then we would be able to stop or prevent muscle wasting," explains the expert in diabetes and obesity Zorzano, head of the "Heterogenic and Polygenic Diseases" lab at IRB.
"We are showing pharmaceutical researchers a new possible therapeutic target for two diseases that seriously impair the quality of lives of those who suffer from them," says the scientist.
Why type 2 diabetic patients lose less muscle than those with type 1
The study also solves a biomedical enigma related to diabetes. Physicians did not understand why patients with type 2 diabetes—who become resistance to insulin or have very low levels of this hormone—are able to maintain muscle mass or minimize muscle wasting compared to patients with type 1 diabetes—who do not produce insulin—who show a clear loss of muscle mass. The IRB researchers demonstrate that the repression of DOR in muscle cells of type 2 diabetic animals allows the maintenance of muscle mass.
"We interpret DOR repression, which occurs naturally, as an adaptation mechanism to preserve muscle mass and to maintain greater muscular strength in type 2 diabetics," explains David Sala, first author of the study, who has recently started a post-doctoral training period at Sanford-Burnham Medical Research Institute, in La Jolla, California.
Besides working with mice, the scientists have performed experiments on biopsies from skeletal muscle of patients with diabetes and patients resistant to insulin, thanks to collaboration with clinicians from the Université Lyon 1, in France, and from the Medical University of Byalistok, Poland, also included among the authors.
The project developed in Dr. Zorzano's lab at IRB has been funded by the Centro de Investigación Biomédica en Red de Diabetes y Enfermedades Metabólicas (CIBERDEM), the Spanish Ministry of Economy and Knowledge, and the European project DIOMED, part of the Interreg-SUDOE programme.
More information: "Autophagy-regulating TP53INP2 mediates muscle wasting and is repressed in diabetes." David Sala, Saška Ivanova, Natàlia Plana, Vicent Ribas,Jordi Duran, Daniel Bach, Saadet Turkseven, Martine Laville, Hubert Vidal, Monika Karczewska-Kupczewska, Irina Kowalska, Marek Straczkowski, Xavier Testar, Manuel Palacín, Marco Sandri, Antonio L. Serrano, Antonio Zorzano. Journal of Clinical Investigation (2014) DOI: 10.1172/JCI72327