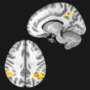
Putting a number on pain

"How much pain are you in?" It's a harder question than many people think. Tools for assessing patients' pain—be they children or adults—rely on perception: a subjective measure that eludes quantification and can change in response to any number of emotional, psychological or physiological factors.
Being able to objectively quantify pain could open the door to better pain management, especially for patients with chronic or neuropathic pain; better anesthetic dosing during surgical procedures; and better understanding of addiction and how to avoid it.
To do so requires measurable markers: physiologic parameters that reliably and quantitatively change during the experience of pain. According to pain researcher David Borsook, Harvard Medical School professor of anaesthesia at Boston Children's Hospital, discovering such markers requires a better understanding of the larger context and of events that trigger pain, a perspective he refers to as "systems neuroscience."
Along with colleague Lino Becerra, HMS associate professor of anaesthesia at Boston Children's, Borsook runs the P.A.I.N. Group—a first-of-its-kind multidisciplinary collaboration between HMS, Boston Children's, Massachusetts General Hospital and McLean Hospital aimed at evaluating long-term changes in children's brain function that can lead to chronic pain.
"In many pain-related conditions, the patient is normal and then something changes that alters their experience of pain," Borsook said. "A twisted ankle could lead to complex regional pain syndrome [CRPS], surgery could lead to postsurgical neuropathy, a concussion can cause debilitating ongoing headaches, and so on. The question is, how do we integrate data from different research domains in such a way as to track the triggers?"
It's a daunting task. To do it means imaging or otherwise measuring changes in brain activity and chemistry associated with different kinds of pain in different contexts, such as neuropathy, addiction, CRPS and migraine; measuring response to different stimuli, such as surgery, brain injury or hormonal activity, and different kinds of treatment, such as psychological, physical or occupational therapy, analgesics and anesthetics; and analyzing the many neurologic circuits and networks involved in sensation, emotion, cognition and interoception, perceptions of the body's internal stimuli.
Connecting the (pain) dots
Bit by bit, though, some pictures are starting to emerge. For instance, functional magnetic resonance imaging (fMRI) data are helping Borsook's team understand and quantify how the activity between different parts of the brain changes during pain.
And, in a paper published this year in Pain, the team highlighted changes in CRPS patients in the functional connections between the amygdala—a brain structure involved in pain, reward, fear and anxiety—and other brain regions that regulate fear.
Stopping pain before it starts
As researchers untangle the complex pathways that fuel chronic pain, they are asking how to take the next step: Stopping the pain it before it becomes chronic.
"Protecting a child's or adult's brain from the changes that take place during chronic pain development could stop that development in the first place," Borsook explained.
One context in which the P.A.I.N. team's work could have major impact is surgery. "There are 29 million surgeries conducted in the U.S. every year," Borsook noted. "About 30 percent of them result in chronic pain."
The team is investigating whether measurements of brain activity taken with near-infrared spectroscopy (NIRS), which measures blood flow and oxygen use, could help anesthesiologists titrate anesthetics more effectively.
"fMRI can measure responses, but NIRS is much more amenable to use in the operating room," Borsook said, pointing to a 2013 paper in Annals of Surgery. "It could let us measure stress and anxiety related to the procedure, look at the effect of the anesthetic itself and look for markers indicating the creation of pain triggers."
Similarly, knowledge of how the brain and hormones interact may give insight into migraine, its relationship to puberty, how to measure it and how to stop it.
"The prevalence of migraine shoots up around the time of puberty, especially in girls," Borsook said. "Why? What are the triggers?"
He and his colleagues recently published a review in Neurobiology of Disease discussing the complex interplay of hormone effects, age- and sex-related physiologic changes and brain function; how that interplay can lower the migraine threshold in girls' brains; and how that migraine-prone state feeds on itself to make women more susceptible to future migraines.
"We suggest that there are a number of important routes of research that may help us better understand how hormones affect the migraine brain," they wrote, such as studying brain function/hormonal relationships and the short- and long-term effects of oral contraceptives on migraine.
For their part, the P.A.I.N. team has already documented connectivity changes in the hypothalamus of migraine patients. As they reported in a PLoS ONE paper, these changes may help explain some autonomic symptoms of migraine, for example, nausea, sweating and feeling of heat or cold.
In discussing a systems approach to pain, Borsook highlighted the need to partner closely across disciplines to truly understand the biology underlying the pain experience.
"Pain is part of many, many diseases," he said. "Processes that alter the healthy brain in children and cause chronic pain produce changes that may affect individuals for life, and as such we have an urgent need to understand and prevent long-term changes. You have to collaborate with people from many biological and medical perspectives in order to draw a clear picture of what those changes are, and how to reverse or prevent them."
More information: "The responsive amygdala: Treatment-induced alterations in functional connectivity in pediatric complex regional pain syndrome." Simons LE, et al. Pain. 2014 May 23. pii: S0304-3959(14)00256-5. DOI: 10.1016/j.pain.2014.05.023.