Stress-related inflammation may increase risk for depression

Preexisting differences in the sensitivity of a key part of each individual's immune system to stress confer a greater risk of developing stress-related depression or anxiety, according to a study conducted at the Icahn School of Medicine at Mount Sinai and published October 20 in the Proceedings of the National Academy of Sciences (PNAS).
Inflammation is the immune system's response to infection or disease, and has long been linked to stress. Previous studies have found depression and anxiety to be associated with elevated blood levels of inflammatory molecules and white blood cells after a confirmed diagnosis, but it has been unclear whether greater inflammation was present prior to the onset of disease or whether it is functionally related to depression symptomology.
Specifically, the new study measured the cytokine IL-6 in non-aggressive mice prior to and after repeated social stress invoked by an aggressive mouse. They found that IL-6 levels were higher in mice that were more susceptible to stress than in "stress-resilient" mice. They also found the levels of leukocytes (white blood cells that release IL-6) were higher in stress susceptible mice before stress exposure. The researchers then validated the increased levels of IL-6 in two separate groups of human patients diagnosed with treatment-resistant Major Depressive Disorder.
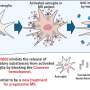
The Mount Sinai study results revolve around the peripheral immune system, a set of biological structures and processes in the lymph nodes and other tissues that protect against disease. Inflammation is a culprit of many disease conditions when it happens in the wrong context or goes too far. Under normal conditions when the immune system perceives a threat (e.g. invading virus), inflammatory proteins called interleukins are released by white blood cells as an adaptive mechanism to limit injury or infection. However, in some instances, the immune system may become hyper responsive to an "insult," leading to chronic dysregulation of inflammatory processes that ultimately cause disease.
"Our data suggests that pre-existing individual differences in the peripheral immune system predict and promote stress susceptibility," says lead author Georgia Hodes, PhD, Postdoctoral Researcher in Neuroscience. "Additionally, we found that when mice were given bone marrow transplants of stem cells that produce leukocytes lacking IL-6 or when injected with antibodies that block IL-6 prior to stress exposure, the development of social avoidance was reduced compared with their respective control groups, demonstrating that the emotional response to stress can be generated or blocked in the periphery."
Evidence in the current study is the first to suggest that Interleukin 6 response prior to social stress exposure can predict individual differences in vulnerability to a subsequent social stressor.
The research team, led by Scott Russo, PhD, Associate Professor of Neuroscience, exposed mice to two social stress models that are translational to social stressors experienced by humans. They measured blood levels of cytokines in non-aggressive mice before and after repeated social defeat stress invoked by exposure to an aggressive mouse for 10 minutes daily for 10 days or after 10 days of witnessing defeat of another mouse, a purely emotional stressor. The researchers classified the non-aggressive mice as susceptible based on a preference to spend more time near an empty cage rather than near a new mouse on a subsequent social interaction test, whereas resilient mice showed the opposite pattern. Interleukin-6 was the only cytokine significantly elevated in susceptible mice compared with unstressed and resilient mice.
As has been witnessed in humans, they found that chronic social subordinations in mice leads to depression-like behavior, including social avoidance, in a subset of mice termed susceptible, whereas resilient mice resist the development of such behavior.
"Interleukin-6 could be a risk factor for the development of depression in vulnerable individuals," says Dr. Russo. "We believe our studies could have significant impact on the development of new antidepressant therapeutics that inhibit IL-6, which may reduce stress-induced relapse in patients with major depressive disorder."
The new study provides experimental evidence that the emotional response to stress can be generated or blocked in the periphery, offering the potential for new forms of treatment for stress disorders and may eventually inform therapeutic strategies to reengineer a patient's immune system to reduce stress vulnerability. Given that stress disorders and inflammation are together associated with increased prevalence of many other chronic diseases, such as heart disease and stroke that are highly comorbid with emotional disturbances, these findings may provide insight into common pathways governing multiple diseases.
Human blood samples used in the study were collected at Mount Sinai and the University of Cambridge.
More information: Individual differences in the peripheral immune system promote resilience versus susceptibility to social stress, PNAS, www.pnas.org/cgi/doi/10.1073/pnas.1415191111