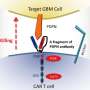
A new weapon in the fight against children's brain tumors
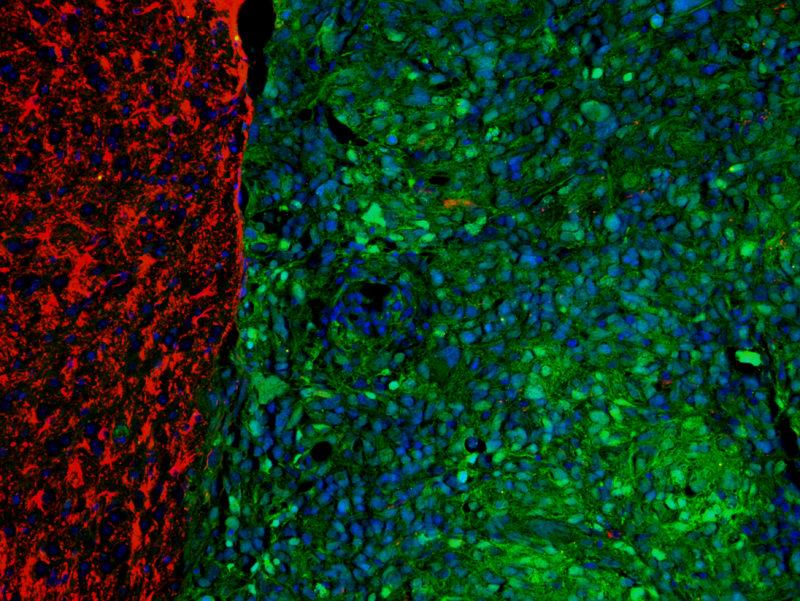
Children with brain cancer may soon get some help from mice with the same disease, thanks to new research from University of Michigan Medical School scientists and their colleagues.
In a new paper in Science Translational Medicine, the U-M team describes how they developed a novel brain tumor model in mice.
The mice have the same genetic problems as those seen in many children with the most dangerous forms of brain cancer. That means the mice should be able to serve as a new test bed for treatments aimed at shrinking children's tumors.
Unlike adults with brain cancer, children cannot receive radiation therapy, so doctors must rely on medications and other strategies. Brain tumors are the leading cause of cancer death in children. A lack of treatment options keeps survival rates low.
"This is exciting because it's the first animal model of pediatric high-grade gliomas, or malignant brain tumors," says Maria Castro, Ph.D., senior author of the paper and a professor in the departments of Neurosurgery and Cell and Developmental Biology at U-M. "The mice carry the genetic mutations found in human tumors, and develop tumors that closely resemble what children and adolescents do."
And unlike previous attempts by others, the model generated at the U-M has a fully functional immune system, which makes it even more alike the children they mimic.
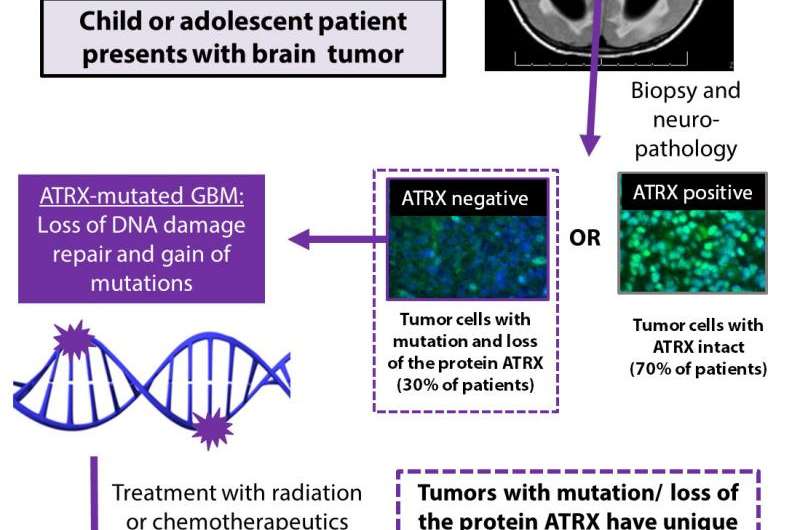
Brain cancer biology
In addition to developing the new genetically engineered mouse model for the form of cancer called glioblastoma multiforme, the researchers made a key discovery about brain tumor biology via the mice. Their work focuses on a protein called ATRX, and its role in helping cells repair damage to DNA. About one-third of children and young adults with brain cancer have ATRX mutations in their cancer cells.
Using a special genetic technique that introduced the same mutation in mice, soon after birth, the scientists were able to generate brain tumors that made less of the ATRX protein. Then, they showed that when the cancer cells didn't make enough ATRX, the cells couldn't join together the two ends of a broken DNA strand.
This genetic instability accelerated tumor growth and reduced the survival of mice that went without treatment.
But in an ironic - and potentially beneficial - twist, the researchers also showed that if they treated the mice's tumors with drugs that damage DNA, they could actually shrink tumors more effectively and improve survival.
DNA-damaging cancer drugs already exist, and are used for other purposes in adults. If further research in the mice bears out, they could soon be tested in children whose brain tumors also show a decrease in ATRX production.
The first author of the study, U-M children's cancer specialist Carl Koschmann, M.D., helps guide the treatment of children with brain cancer at U-M's C.S. Mott Children's Hospital. He also studies brain cancer at the basic cell level in the Castro laboratory.
"We are very excited about this tumor model as it mimics the developmental environment of a pediatric or adolescent human brain tumor," he says. "We desperately need new therapies for pediatric GBM patients, as less than 20 percent of children diagnosed with GBM will survive five years. We currently base their treatment on a regimen designed for adult patients with GBM, which are very different tumors at the molecular level. Our mouse model has given us a great step towards developing targeted therapies to specific changes found in pediatric and adolescent GBM."
Accelerating discovery
Dr Castro's team at U-M, and their colleagues on teams at the Johns Hopkins School of Medicine, the University of Rochester, and the Institute of Cancer Research in London have been working toward this goal for several years.
A crucial aspect of the mouse model development was the ability to use what's called the "Sleeping Beauty" technique of inserting genes into stem cells in the brain of newborn mice. This allows their brain to develop normally, but also triggers the development of cancer by adding mutated ATRX genes and other genes known to be involved in cancer.
They also looked at genetic data on several hundreds of adult and pediatric brain tumors from around the world. That helped them confirm that mutations in the gene that directs cells to make ATRX are responsible for making the tumors genetically unstable.
Personalizing treatment for brain tumors based on an individual's ATRX mutation status is still a concept, not a reality. But the researchers believe their mouse model and the close collaboration with pediatric brain cancer treatment teams at Mott Hospital will accelerate the ability to do so.
More information: Science Translational Medicine (2016). DOI: 10.1126/scitranslmed.aac8228