Nuclear DNA gets cut and activates immune system to attack cancer cells
The conventional wisdom about cancer cells is that they are masters of camouflage, invisible to the immune system. However, occasionally, the immune system is alerted to the presence of a cancer cell and springs into action to attack it.
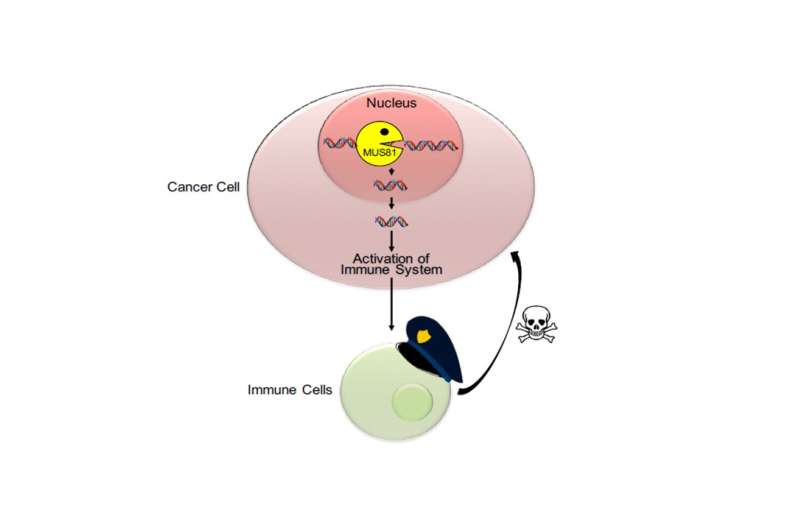
A new study led by Assistant Professor Stephan Gasser of the Department of Microbiology and Immunology at the National University of Singapore's Yong Loo Lin School of Medicine has identified a snitch that "reveals" cancer cells to the immune system. Published online on 10 May 2016 in the prestigious journal Immunity, the study found that when an enzyme called MUS81 cuts DNA in the nucleus, the DNA is not degraded, but rather moves to the cytoplasm in cancer cells. DNA being in the wrong place alerts the immune system, triggering it to attack cancer cells.
Dr Samantha Ho, the first author of the article, and colleagues in the laboratory of Asst Prof Gasser found that out-of-place DNA in cancer cells activates the immune system by producing a substance called interferon that activates immune cells called macrophages and T cells to kill cancer cells. MUS81 plays an essential role in this killing of cancer cells because nuclear DNA was not cut in cancer cells that lacked the enzyme and no activation of the immune system was observed in these cells.
Although most of the work has been carried out using in vivo studies, Asst Prof Gasser has been collaborating with Dr Joanne Ngeow at the National Cancer Centre Singapore to characterise the process in different types of human tumours. Their preliminary findings indicate that MUS81-induced movement of DNA to the cytosol also occurs in human cancer cells, including prostate cancer, breast cancer, colorectal cancer, uterine cancer, leukemia, and melanoma cells.
Discovering this process in cancer cells has wider implications beyond just describing a phenomenon. Several of the current chemotherapies against cancer activate MUS81 and may therefore trigger a stronger immune response. These therapies could enhance the effects of novel cancer immunotherapies when used in combination, resulting in better health outcomes for cancer patients.