Smart molecules trigger white blood cells to become better cancer-eating machines
A team of researchers has engineered smart protein molecules that can reprogram white blood cells to ignore a self-defense signaling mechanism that cancer cells use to survive and spread in the body. Researchers say the advance could lead to a new method of re-engineering immune cells to fight cancer and infectious diseases. The team successfully tested this method in a live cell culture system.
The work was led by bioengineering professors Peter Yingxiao Wang and Shu Chien with collaborating professors Victor Nizet and Xiangdong Xu, all at the University of California San Diego, along with researchers from the University of Illinois at Urbana-Champaign. The team published their work this month in Nature Communications.
The smart proteins, called "iSNAPS" (integrated sensing and activating proteins), are designed to detect precise molecular signals in live cells and in response, act upon those signals to enable the cells to fight disease or perform other beneficial functions. This study is the first to demonstrate how both sensing and activating capabilities can be combined into a single molecule, Wang said.
The researchers inserted their iSNAPS into a type of white blood cells called macrophages and demonstrated that they dramatically enhanced the macrophages' ability to engulf and destroy rapidly dividing cancer cells.
Macrophages are white blood cells that play a significant role in the immune system. Part of their task is to remove foreign particles and harmful organisms such as pathogens and cancer cells by digesting them. When a macrophage binds to a cancer cell or other foreign invader, surface proteins on the macrophage called Fc gamma receptors send out an "eat me" signal that prompts the macrophage to engulf and destroy the invader.
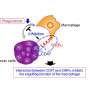
However, cancer cells have a special protection mechanism that contributes to their deadly disease potential. They have a surface protein called CD47 that interacts with the macrophage's SIRP-alpha surface protein to send out a negating "don't eat me" signal.
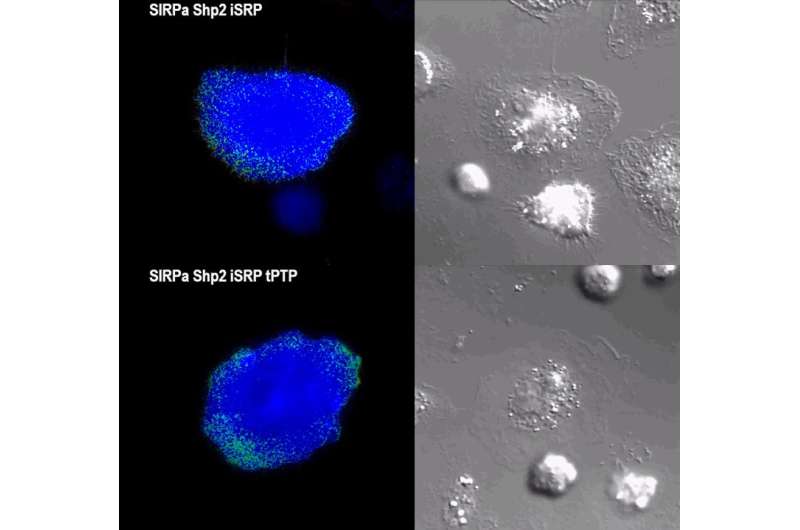
The secret to getting the iSNAP technology to work involves reconfiguring the battleground between the cancer cells and the immune system. The iSNAPS essentially rewire macrophages to override this "don't eat me" signal and interpret it as an "eat me" signal. The iSNAPs have a sensing component that detects the key molecular event that occurs inside a macrophage when its SIRP-alpha surface protein interacts with CD47 on the cancer cell. In response, the iSNAPS have an activating component that immediately transforms to produce a green/yellow light signal, giving researchers a way to visualize the molecular activity through a microscope. The activating component is also triggered to release an enzyme that initiates a cascade of events that enables the macrophage to engulf the cancer cell. "What's noteworthy is that this response time is very fast—we believe it happens within seconds to minutes" Wang said.
In their experiments, the researchers mixed their engineered macrophages with cancer cells in culture dishes and observed the activity through a microscope. The macrophages were able to engulf most of the cancer cells tested. As a control experiment, the researchers used macrophages containing disabled iSNAPS, which have sensing capability but no activating capability. They observed that these macrophages could bind and detect the presence of the cancer cells but not eat them.
Wang noted that the iSNAPS design could in principle be modified for other uses, such as re-engineering immune cells to kill bacteria. They could also be applied to other immune cell types such as T cells for multi-pronged cancer therapy. Moving forward, the team is planning to test the iSNAPS in mice to see how they would perform in vivo. The researchers are also interested in studying whether the iSNAPS can be harnessed to enhance other native cellular functions to correct various disease pathologies.
More information: Jie Sun et al, Engineered proteins with sensing and activating modules for automated reprogramming of cellular functions, Nature Communications (2017). DOI: 10.1038/s41467-017-00569-6