Screening all donated blood for Zika virus is not cost-effective in the United States
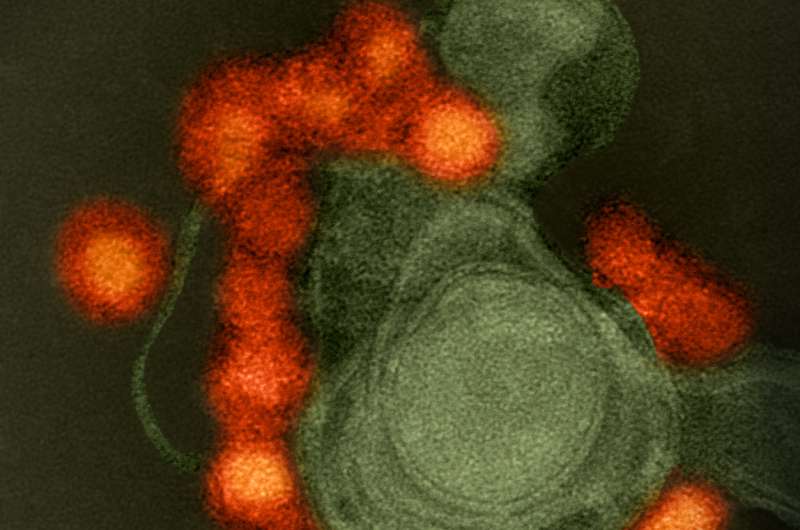
Universal screening of individual blood donations for Zika virus, which began in 2016, was not cost-effective in the 50 states during the first year. Widespread screening would only be cost-effective in the high mosquito season in Puerto Rico and never in the 50 states. Findings from a microsimulation study are published in Annals of Internal Medicine.
The Zika epidemic of the Americas beginning in 2015 is the largest outbreak to date. Because Zika virus is associated with severe illness, such as Guillain-Barre syndrome, and potentially devastating birth defects, such as microcephaly, the U.S. Food and Drug Administration (FDA) implemented measures to protect transfusion recipients from infection. In 2016, the FDA began requiring universal individual donation nucleic acid testing (ID-NAT) of donated blood for Zika virus in U.S. states and territories. Universal screening is still required today, although mini-pool NAT (MP-NAT) is permitted as of July 2018. However, the effectiveness and cost-effectiveness of these measures had not been evaluated previously.
Researchers from Stanford University, Vitalant Research Institute, and the American Red Cross used a microsimulation to estimate the effectiveness and cost-effectiveness of universal ID-NAT, universal mini-pool NAT, and alternative Zika virus screening policies in Puerto Rico and the 50 states. The microsimulation captured Zika-related harms to transfusion recipients, sexual partners, and their infants to weight the cost/benefit of universal screening. They found that during the first year of testing, screening was cost-effective only in the high mosquito season in Puerto Rico, and no evaluated screening policy was cost-effective in the 50 states. Because the Zika epidemic is largely over, screening policies are much less cost-effective today than during the period of their analysis. These findings suggest that revisiting the universal blood screening policy would be warranted. However, the authors note that many other considerations should inform blood safety policies in addition to cost-effectiveness.
More information:
Study: http://annals.org/aim/article/doi/10.7326/M18-2238
Editorial: http://annals.org/aim/article/doi/10.7326/M18-3527