Scientists discover key enzyme in breast cancer proliferation, treatment resistance
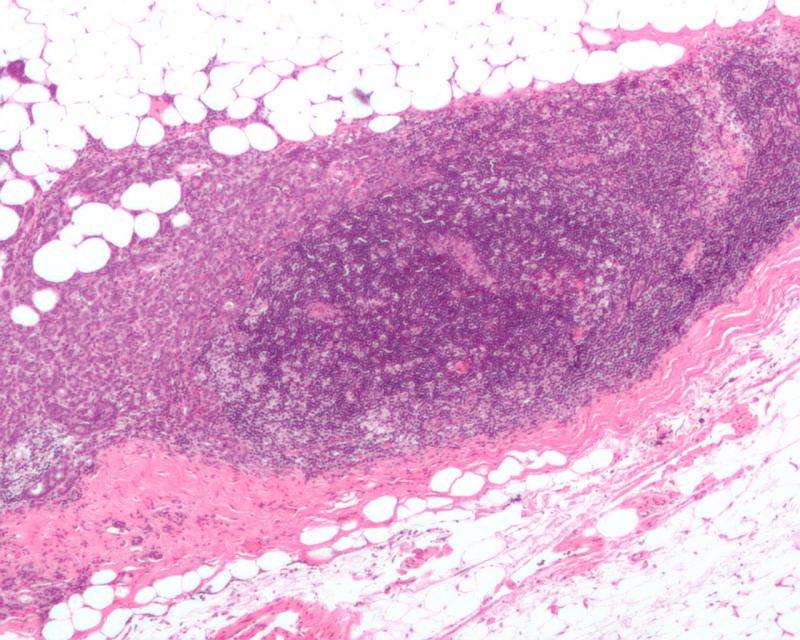
Basal-like breast cancer is the most aggressive and difficult-to-treat subtype of breast cancer, and it largely overlaps with the triple-negative classification of the disease. Patients are in dire need of improved therapies that attack the underlying cellular features of these types of breast cancer.
Now scientists at the UNC School of Medicine and the UNC Lineberger Comprehensive Cancer Center have uncovered a possible reason why these cancers are so aggressive. In lab experiments, the researchers found that an enzyme called USP21 promoted proliferation of basal-like breast cancer and is upregulated in a significant percentage of patient tumors.
The discovery, published in Cell Reports, offers researchers a much-needed target for new therapies to battle aggressive subtypes of breast cancer.
"We think USP21 could not only drive basal-like breast cancer in patients, but could represent a new, future target for therapeutic intervention," said senior author Michael Emanuele, Ph.D., associate professor of pharmacology and UNC Lineberger member. "We also think targeting USP21 could sensitize cancer cells to therapies already in clinical use to treat patients with this disease."
In cancer cells, proteins called transcription factors control the rate at which genetic information is copied from DNA to messenger RNA inside cells. This transcription is crucial for the proper completion of the cell cycle and cell proliferation, including for cancer cells. One of these transcription factors is called FOXM1, which has been found in significant quantities in basal-like breast cancer (BLBC). Despite its importance in normal and cancer cell cycles, scientists have lacked a complete understanding of the mechanisms that regulate FOXM1.
Using an RNA interference-based screening technique to determine regulators of FOXM1 abundance, Emanuele and colleagues found that the enzyme USP21 increased the abundance and stability of FOXM1. The more USP21 in cells, the more FOXM1 was protected during the cell cycle. When the researchers depleted USP21, they noticed a major decrease in the proteins involved in FOXM1's transcriptional network and a significant delay in cell cycle progression.
In their paper, first author Anthony Arceci, Ph.D., a graduate research assistant in the Emanuele lab, and colleagues show that USP21 depletion sensitized basal-like cancer cells and tumors to paclitaxel—a front-line therapy in BLBC treatment. USP21 is the most frequently amplified enzyme of its class in BLBC patient tumors, and its amplification coincided with the upregulation of FOXM1. This research finding suggests USP21 plays a major role in the proliferation and potential treatment of FOXM1-high, USP21-high basal-like cancer.
"We found that USP21 is commonly upregulated in basal-like, triple-negative breast cancers," Emanuele said. "We think it's possible to develop a drug to inhibit USP21 in the future, to trick the cancer cells into destroying FOXM1 and stopping cancer cells from continuing to grow and proliferate."
The Emanuele lab is further testing these findings is additional animal models of breast cancer to validate USP21 as a potential drug target. The lab also plans to test compounds to inhibit USP21.
More information: Cell Reports (2019). DOI: 10.1016/j.celrep.2019.02.054