Making cancer stem cells visible to the immune system
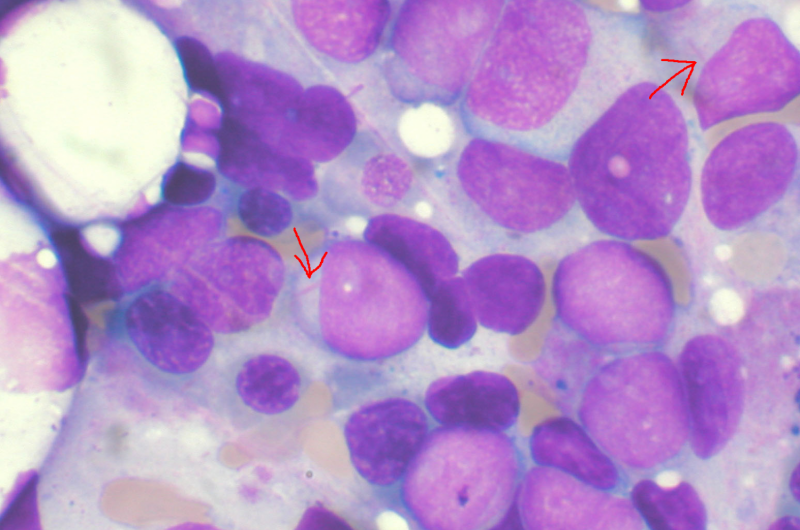
Leukemia stem cells protect themselves against the immune defense by suppressing a target molecule for killer cells. This protective mechanism can be tricked with drugs. In the journal Nature, scientists from Basel, Tübingen and Heidelberg describe the new therapeutic approaches that can possibly be derived from these results.
Patients with acute myeloid leukemia (AML) often relapse after apparently successful treatment. Leukemia stem cells that survive the therapy are responsible for the return of the disease. Scientists can partially explain this phenomenon: The stem cells have protective mechanisms that make them resistant to chemotherapy. But how do they manage to escape the immune defense?
A team of scientists from the Universities of Basel and Tübingen, the German Cancer Research Center (DKFZ), the Heidelberg Institute for Stem Cell Technology and Experimental Medicine (HI-STEM) and the German Cancer Consortium (DKTK) have now investigated this phenomenon and discovered a surprising mechanism.
The researchers analyzed the leukemia cells of 175 AML patients and found that the cancer stem cells suppress the NKG2D-L proteins on their surface. These proteins enable the natural killer cells (NK cells) to recognize damaged and infected cells as well as cancer cells and kill them if necessary. In this way, the leukemia stem cells escape destruction by the immune system. Leukemia cells without stem cell properties, on the other hand, present these target molecules on their surface and are therefore kept in check by the NK cells.
In mice to which AML cells from patients had been transferred, the researchers showed that while the normal AML cells (without stem cell properties) were controlled by the NK cells, the NKG2D-L-negative leukemia stem cells escaped the killer squad. "Such a connection between stem cell properties and the ability to escape the immune system was unknown until now," said Claudia Lengerke from the University Hospital of Basel and the University of Basel. "An essential mechanism of this immune resistance in leukemia stem cells is apparently the suppression of danger signals such as NKG2D-L on the cell surface," added Helmut Salih from the University Hospital of Tübingen and the German Cancer Consortium DKTK.
What is behind this extraordinary protective mechanism? The scientists noticed that leukemia stem cells produce a particularly high amount of PARP1, an enzyme that apparently blocks NKG2D-L production. Preclinical experiments with mice to which human leukemia cells had been transferred showed that PARP1 actually plays an important role in immune escape: If these animals were treated with drugs that inhibit PARP1, the leukemia stem cells again expressed NKG2D-L on their surface—and were then recognized and eliminated by NK cells.
Cancer therapies involving the immune system have been successfully applied for many years in the form of allogeneic stem cell transplantation in AML patients in certain disease situations. In recent years, further novel immunotherapeutic approaches have been developed which are currently being clinically tested. "Our results show how cancer stem cells cleverly trick the immune system. The elucidation of the underlying mechanism now makes it possible to counterattack," says Andreas Trumpp, German Cancer Research Center and HI-STEM.
The results provide the basis for the possibility of combating malignant leukemia stem cells by combining PARP inhibitors with active NK cells. The scientists involved are now planning to evaluate this approach in a clinical study.
More information: Absence of NKG2D ligands defines leukaemia stem cells and mediates their immune evasion, Nature (2019). DOI: 10.1038/s41586-019-1410-1