This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
trusted source
proofread
Cancer cells may sense immune surveillance and actively adapt
Scientists have proposed a theory for how cancer cells might actively adapt themselves to the immune system to become resistant to immunotherapy, a study published today (April 25) in eLife reports.
Their theory suggests that as a population of cancer cells evolves and adapts in response to being recognized and destroyed by the immune system, immune recognition and environmental conditions determine the difficulty with which a future disease may be targeted with different treatment.
Treatments that harness the body's own immune system against cancer (immunotherapies) hold the promise of more durable remission from the disease. By targeting molecular "flags" on the surface of tumor cells called tumor-associated antigens (TAAs), it becomes possible to alert the body's immune system to their presence—potentially for many years.
Unfortunately, just as tumors find compensatory mechanisms to adapt to chemotherapy, cancer cells can also find ways to evade recognition by the immune system. But while drug resistance might be problematic for conventional therapies, when cancer cells adapt to avoid immune recognition, they lose and gain TAAs, and these new antigens could potentially be targeted by new immunotherapies.
"It had previously been assumed that cancer cells adapt to being recognized by the immune system in a passive way, rather than sensing the surrounding immune environment and actively adapting," explains co-author Jason George, Assistant Professor in the Department of Biomedical Engineering, Texas A&M University, Texas, U.S.
"However, previous experiments have demonstrated that the level of cancer evasion can be fine-tuned by malignant cells sensing environmental and immunological stresses. In responding to stress, cancer cells can adapt by picking up mutations and by altering the level of otherwise rare proteins, for example, to survive. This can lead to changes in the antigen signatures present on cancer cells that the immune system is able to recognize, and tracking these modifications could reveal new vulnerabilities that can be therapeutically targeted."
Under surveillance from the human immune system, cancer cells are either eliminated, escape the immune system or reach an equilibrium—where the cancer coexists with the immune system over a long period of time. All these outcomes depend on a complex interplay between immune recognition and cancer evolution, and the resulting effects of a cancer adaptive evasion strategy on subsequent disease progression is largely unknown.
To address this, the team developed a mathematical model to quantify the aggressiveness of a cancer cell population's evolutionary strategy when faced with different immune environments.
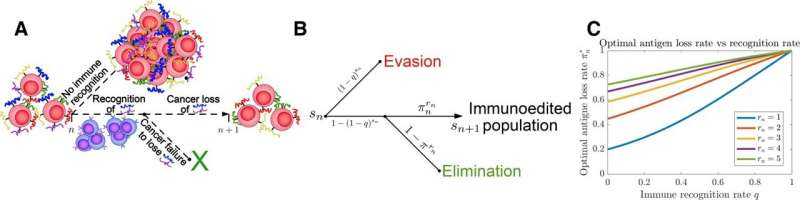
The model, called Tumor Evasion via adaptive Antigen Loss (TEAL), consists of a population of cancer cells that are targeted over time by a recognizing system—that is, the immune system. If cancer cells use a passive strategy, the cancer population does not change the rate at which it tries to evade the immune system over time. By contrast, in an active evasion strategy, the cancer population possesses key information—for example, the number of TAAs it has, and the level to which immune cells are actively targeting TAAs—and bases its strategy on these insights.
The team mathematically modeled and solved for the dynamical behavior exhibited by both strategies—passive and active evasion tactics—and then tested them with different immune environments over time, ranging from a hostile immune environment with a large number of immune cells recognizing all TAAs, to a less hostile environment with fewer cells recognizing the TAAs.
As the authors predicted, cancer cell populations adopting an active evasion strategy outperformed their passive counterparts, dramatically increasing the frequency at which cancer populations ultimately escape the immune system. However, although these populations evaded immunity, they paid a penalty in the form of an increased number of mutations and/or transcriptional alterations, which affect the overall TAA profile of the cell population.
The model also predicted that cancer cells in a tumor-promoting immune environment would become unstable because they gain and lose TAAs, which could explain why solid tumors often have "hot" and "cold" spots that are responsive or unresponsive to immunotherapy, respectively.
"Actively adapting cancers are by design more difficult to treat. But our model predicts that in some cases, the cancer populations pay a penalty for surviving against immune recognition today that may then be therapeutically targeted tomorrow," says George. "This early work motivates an intriguing research direction for identifying optimal therapeutic strategies against adaptive or 'smart' diseases like cancer, and they will no doubt benefit from mathematical modeling."
The model provides key insights that the authors say will be essential in realizing the potential of immunotherapy for keeping individual patients' tumors at bay for many years.
"Defeating a highly adaptive cancer population has provided a persistent challenge to researchers and clinicians. Progress will be enabled by fundamental discoveries on cancer behavior, and by concomitant additional insights into cancer evasion," says co-author Herbert Levine, Adjunct Professor of Bioengineering at, Rice University, Houston, U.S., and Distinguished Professor of Physics and Bioengineering at Northeastern University, Boston, U.S. "The possibility that cancer population-level strategies can be smart enough to sense the level of immune recognition threat could have a radical effect on our optimal treatment approach."
More information: Jason T George et al, Optimal cancer evasion in a dynamic immune microenvironment generates diverse post-escape tumor antigenicity profiles, eLife (2023). DOI: 10.7554/eLife.82786