This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
trusted source
proofread
Impaired verbal memory found to increase psychiatric patients' risk of hospitalization
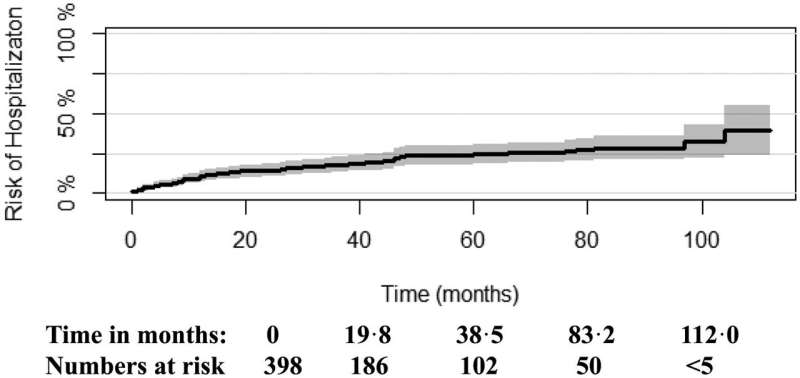
Memory plays a crucial role in people's social and working lives. Now, new research shows that verbal (i.e. linguistic) memory also determines whether psychiatric patients diagnosed with bipolar disorder or depression are at risk being hospitalized or readmitted to a psychiatric ward.
"It has long been known that patients who have previously been hospitalized with major depression or bipolar disorder often have impaired memory. But it was believed that it was the severity of the illness itself that played a role in the poor memory. Now we can see that the arrow also points the other way," says Kamilla Miskowiak, professor at the Department of Psychology at the University of Copenhagen.
In the new study, Kamilla Miskowiak, in close collaboration with senior researcher Anjali Sankar and a number of other researchers from the Neurobiological Research Unit at Rigshospitalet and the UCPH, followed 518 patients over a number of years, all of whom have previously undergone the same cognitive tests in other studies.
Combined with data from Statistics Denmark, the researchers have used the previous studies to see to what extent the patients' verbal memory and so-called executive functions, such as the ability to plan and problem-solve, affect the risk of being hospitalized in a psychiatric ward.
The conclusion is clear: "Poor verbal memory in itself increases the risk of psychiatric hospitalization. This is evident when we adjust for previous hospitalization, severity of illness, depression symptoms and other factors that we know are important," explains Kamilla Miskowiak.
Nearly double the risk of hospitalization
The study concludes that there is an approximately 84 percent increased risk of being admitted to a psychiatric ward if you have previously had a clinically significant impairment in the ability to learn and remember verbal information.
The study cannot say for sure why this verbal memory impairment increases the risk. But according to Kamilla Miskowiak, it may be related to the fact that patients often find it more difficult to remember their medication and to keep up with the demands of their everyday life, which in turn can lead to stress.
"We know that stress is a major risk factor for relapse. And many people with mental health problems are already struggling to stay afloat. So being exposed to the additional stress of verbal memory impairment can increase the risk of new severe depressions or manias that require hospitalization."
Conversely, the study finds no significant association between impaired executive function and increased risk of hospitalization. And patients with impaired cognitive function do not appear to fare significantly worse on social parameters such as employment, cohabitation and marital status.
However, the researchers found that poor executive function was associated with a 51 percent reduced likelihood of having achieved the highest level of education (polytechnic and university). Reduced ability to plan and implement problem-solving strategies during studies may hamper educational achievement and vice versa, says Kamilla Miskowiak.
Call for new treatment methods
But above all, it is key knowledge that poor verbal memory itself increases the risk of psychiatric hospitalization among people with mental illness. According to Kamilla Miskowiak, this means that more attention should be paid to impaired memory in psychiatric treatment, which currently has a limited focus on cognitive skills.
"It is not enough just to treat patients' symptoms of depression or mania, for example. We also need to work on strengthening their memory and other cognitive functions as soon as they are symptom stable," she says.
"About half of patients with recurrent depression or bipolar disorder have persistent problems with memory and other cognitive functions. This calls for both more systematic cognitive screening and new treatment approaches."
The study titled "Association of neurocognitive function with psychiatric hospitalization and socio-demographic conditions in individuals with bipolar and major depressive disorders," is published in eClinicalMedicine.
More information: Anjali Sankar et al, Association of neurocognitive function with psychiatric hospitalization and socio-demographic conditions in individuals with bipolar and major depressive disorders, eClinicalMedicine (2023). DOI: 10.1016/j.eclinm.2023.101927


















