This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
trusted source
proofread
Study optimizes patient-specific stem cell-based therapy for Parkinson's disease
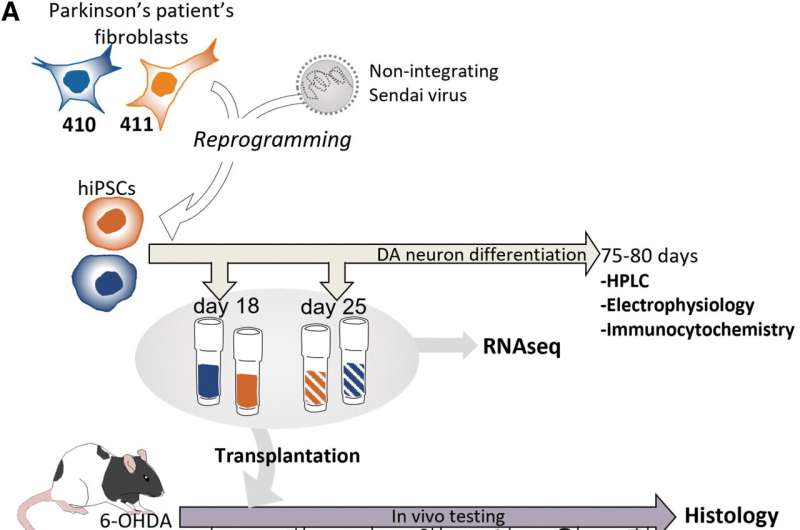
Scientists from Scripps Research and Cardiff University have made key discoveries in support of a new stem cell-based therapy for Parkinson's disease. The approach, called an autologous therapy, uses induced pluripotent stem cells (iPSCs)—made from a patient's own skin or blood cells—to replace the neurons in the brain that are lost in Parkinson's. Transplants of a person's own cells eliminates the need for immunosuppression.
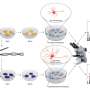
In a new study, the researchers used iPSCs made from the skin cells of two people with Parkinson's disease to make young neurons that were successfully transplanted into a rat model with the disease. They used the animal model to pinpoint exactly at what stage of development the iPSC-derived neurons should be transplanted to become mature neurons that can reverse signs of disease in the rat brain.
The research, published in Stem Cells and Development, is a crucial step forward for clinical trials of autologous iPSC-derived neurons in human patients with Parkinson's disease.
"This paper reports important progress toward development of an autologous cell replacement therapy for Parkinson's disease," says senior author Jeanne Loring, Ph.D., professor emeritus and director of the Center for Regenerative Medicine at Scripps Research and co-founder of Aspen Neuroscience, Inc. "These results give us confidence that personalized therapy is feasible for Parkinson's disease.
For over a decade, researchers have been developing methods for using iPSCs—which can form any cell type in the body—to treat a variety of diseases characterized by defective or missing cells. People with Parkinson's disease have lost neurons that produce a chemical messenger called dopamine in the brain.
The resulting low levels of dopamine lead to the symptoms of Parkinson's, which are typically tremors and slow movement. There is currently no cure for the disease, and there are only limited options for controlling symptoms. Nearly 90,000 people are diagnosed with Parkinson's each year, and 10 million people worldwide are living with the disease.
Today, clinical trials are already underway using stem cells to replace dopamine-producing neurons in the brains of people with Parkinson's disease, but the trials all use unmatched cells from the lab or a donor, rather than cells from a patient's own body.
"When you transplant neurons derived from someone else's cells, those cells will be rejected by the immune system, requiring the use of immunosuppressive drugs that are often not well tolerated," says Loring.
Loring and co-senior author Mariah Lelos, from Cardiff University, instead focused on iPSCs derived from patients. In the new work, they wanted to find the optimal developmental stage for transplanting the precursor neurons.
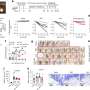
They found that transplants using two different stages of early-neuron progenitors could both be successfully grafted into the brain. However, they were surprised to discover that only one stage, the earlier precursors, were effective in reversing symptoms of Parkinson's disease. Looking more closely, they found the difference: The younger cells were better able to connect with other neurons.
When the scientists examined the cells to determine what genes were being expressed by each of the neuronal precursor stages, they discovered that many genes associated with neuronal differentiation were turned off in the younger cells and turned on in the older ones.
"At this earlier time point, the cells are poised to become neurons, and when they are put into the brain, they receive the signals to turn on those genes and finish their development. This allows them to make connections with the host," explains Lelos. "If they're farther along in development, they no longer respond to those initial developmental signals."
"Knowledge of which genes are turned on in neuronal precursors that are in the optimal developmental state to treat Parkinson's can help researchers screen cells before transplanting them into patients," Loring adds. "The gene expression analysis should greatly improve the probability of successful transplants," she says.
The findings may also be a boon to researchers using iPSCs to develop therapies for other diseases, including Huntington's disease, age-related macular degeneration and heart failure.
In addition to Loring and Lelos, authors of the study include Andres Bratt-Leal, Ha Tran, Roy Williams, David Stouffer, Irina Sokolova and Pietro Sanna of Scripps Research; Rachel Hills of Cardiff University; and independent bioinformatics consultant Jim Mossman.
More information: Rachel Hills et al, Neurite Outgrowth and Gene Expression Profile Correlate with Efficacy of Human Induced Pluripotent Stem Cell-Derived Dopamine Neuron Grafts, Stem Cells and Development (2023). DOI: 10.1089/scd.2023.0043