This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
trusted source
proofread
Researchers study signaling pathway in adipose tissue as a means to curb diabetes, obesity
Researchers at Vanderbilt University Medical Center have uncovered a potential new way to help curb the rapidly rising worldwide prevalence of metabolic disorders, including obesity and diabetes.
Their investigation, reported recently in the Journal of Clinical Investigation, focused on a signaling pathway in adipose (fatty) tissue that is important in the control of metabolism, and which, if tweaked the right way, could enhance insulin action and block the obesity-inducing effects of a high-fat diet.
The paper's senior authors, Heidi Hamm, Ph.D., and Sheila Collins, Ph.D., are known internationally for their research on G proteins and G protein-coupled receptors (GPCRs).
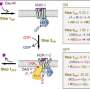
Consisting of two subunits, Gα and Gβγ, G proteins are intracellular molecular "switches" that translate and transmit GPCR signals. Embedded in the membranes of nearly every cell, GPCRs are the most common conduit for signaling pathways found in nature. Two-thirds of all drugs on the market today target them.
Hamm, the Aileen M. Lange and Annie Mary Lyle Professor of Cardiovascular Research, is a former chair of Pharmacology at Vanderbilt. Collins, professor of Medicine in the Division of Cardiovascular Medicine, is an expert on adrenergic receptors, a type of GPCR activated by two neurotransmitters, norepinephrine and epinephrine.

Previously Hamm and her colleagues have shown how the Gβγ subunit of an "inhibitory" G protein prevents intracellular vesicles containing neurotransmitters from fusing to the cell membrane and spilling their contents into the synapse, the extracellular space between nerve cells.
Gβγ inhibits this process, called exocytosis, by binding to SNAP25, one of three proteins in the SNARE complex that is a key regulator of vesicle fusion. The researchers found that when SNAP25 was altered so it could no longer bind to Gβγ, the vesicle fusion "brake" was released.
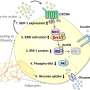
For the current study, Hamm collaborated with Collins, whose lab has identified several signaling pathways in adipocytes (fat-containing cells) that are important for blood glucose control, energy balance (calories consumed versus calories burned), and thermoregulation, which maintains a steady internal body temperature.
The researchers hypothesized that the Gβγ-SNARE interaction blocks vesicle fusion and the release of norepinephrine. This, in turn, impairs the ability of insulin to trigger glucose uptake by body tissues, thereby contributing to metabolic abnormalities characteristic of obesity and Type 2 diabetes.
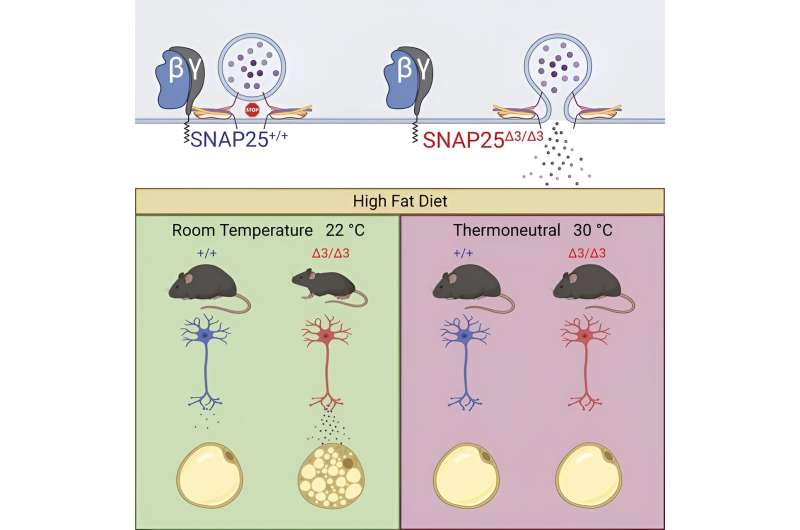
Led by Ryan Ceddia, Ph.D., a postdoctoral fellow in the Collins lab, and Zack Zurawski, Ph.D., a postdoctoral fellow and former graduate student in the Hamm lab, the researchers investigated the impact of a high-fat diet in mice carrying the altered SNAP25 protein, compared to mice with the normal protein.
Mice with the normal SNAP25 gained weight rapidly while on the high-fat diet, whereas those that carried the altered protein were "markedly resistant" to weight gain. Mice with altered SNAP25 also had amplified norepinephrine release, less appetite, and better control of their blood glucose levels suggestive of increased insulin sensitivity.
This discovery provides further evidence that the interaction between Gβγ and SNARE is a negative regulator of exocytosis in the central nervous system and in neurons of the autonomic nervous system, which regulates involuntary physiological functions including energy balance, insulin secretion, and thermoregulation.
Developing drugs that target the Gβγ-SNARE interaction "could be an interesting alternative to directly targeting the GPCRs themselves, given the broad improvements in food intake (and) insulin action," the researchers concluded.
More information: Ryan P. Ceddia et al, Gβγ-SNAP25 exocytotic brake removal enhances insulin action, promotes adipocyte browning, and protects against diet-induced obesity, Journal of Clinical Investigation (2023). DOI: 10.1172/JCI160617