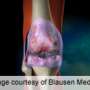
Is zinc the missing link for osteoarthritis therapies?
Osteoarthritis is a leading cause of disability, characterized by the destruction of cartilage tissue in joints, but there is a lack of effective therapies because the underlying molecular causes have been unclear. A study published by Cell Press February 13th in the journal Cell reveals that osteoarthritis-related tissue damage is caused by a molecular pathway that is involved in regulating and responding to zinc levels inside of cartilage cells. A protein called ZIP8 transports zinc inside these cells, setting off a cascade of molecular events that result in the destruction of cartilage tissue in mice. The findings could lead to a new generation of therapies for osteoarthritis.
"No evidence available to date clearly indicated that zinc plays a causal role in osteoarthritis," says senior study author Jang-Soo Chun of the Gwangju Institute of Science and Technology. "In our study, we revealed the entire series of molecular events in the osteoarthritis zinc pathway, from zinc influx into cells to cartilage destruction."
When the cartilage breaks down in osteoarthritis, the bones rub together, causing pain, swelling, and stiffness. This tissue destruction is caused by proteins called matrix-degrading enzymes, which are produced by cartilage cells and are the key culprits responsible for degrading the extracellular matrix—the structural support system that surrounds cells and holds them together. Because matrix-degrading enzymes require zinc to function, Chun and his team suspected that zinc levels inside of cartilage cells may play a role in osteoarthritis.
To test this idea, the researchers first examined cartilage from osteoarthritis patients as well as a mouse model of the disease. They found abnormally high levels of a protein called ZIP8, which is embedded in the plasma membrane of cartilage cells and is involved in transporting zinc inside of these cells from the outside environment. Zinc influx through ZIP8 activated a protein called metal-regulatory transcription factor-1 (MTF1), which in turn increased levels of matrix-degrading enzymes in cartilage cells. Through genetic experiments in mice, the researchers showed that this zinc-ZIP8-MTF1 pathway plays a key role in causing osteoarthritis-related cartilage destruction.
"Our findings suggest that local depletion of zinc or pharmacological inhibition of ZIP8 function or MTF1 activity in cartilage tissue would be effective therapeutic approaches for the treatment of osteoarthritis," Chun says. "We are hopeful that this research will lead to the discovery and rapid development of novel drugs to suppress the progression of this debilitating disease."
More information: Cell, Kim et al.: "Regulation of the catabolic cascade in osteoarthritis by the zinc axis." dx.doi.org/10.1016/j.cell.2014.01.007