Scientists find molecular 'switch' for allergic asthma treatment

A team of Russian scientists has identified the role of the interleukin-6 molecule in the development of allergic asthma. It may comprise a new target for the treatment of this disease. The results are published in Frontiers in Immunology.
About 300 million people worldwide suffer from asthma, one of the most common chronic lung diseases in developed countries. Asthma is considered to be caused by an inadequate response of the immune system to allergens: pollen, herbs, mold, fungi, animal fur or dust mites. This leads to chronic inflammation, narrowing bronchi and respiratory failure. The task of immune scientists is to figure out which internal signals and which cell types direct the this immune response in asthma. Understanding the "molecular language" of cell communication based on cytokines may help to control the immune response by blocking "inadequate" signals and switching the course of the disease from severe to mild.
Clinical studies of sputum samples from patients with bronchial asthma show a high content of interleukin-6, one of the key indicators of inflammatory processes in the body. Therefore, scientists from the laboratory of the molecular mechanisms of immunity of Engelhardt Institute of Molecular Biology in Moscow wondered which immune cells produce it and how its blockage would affect the course of the disease.
"One of the directions in the study of the language of cytokines consists in correlating their useful and disease-causing signals with specific types of producer cells. This paradigm has been formed over the last 10 to 15 years while studying another molecule, the tumor necrosis factor," says Sergey Nedospasov. "For example, in rheumatoid arthritis, tumor necrosis factor molecules from macrophages trigger inflammation, while molecules produced by lymphocytes, on the contrary, can suppress them. We assumed that similar patterns can be found for interleukin-6."
Experiments were performed on unique genetically modified mice in which interleukin-6 production was turned off in a specific type of immune cell: dendritic cells (representing alien objects to T-lymphocytes) or macrophages (cells that absorb alien objects). To induce asthma, mice were injected with dust mite extract. This allergen is most often responsible for asthma in humans.
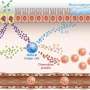
"Just like humans, a mouse has regular contact with dust and dust mites. So this can lead to irritation of the mucous membranes of the respiratory tract and activation of specialized cells of the immune system, T-helper cells of the second type. They help fight allergies and attract inflammatory immune cells to the affected tissues: eosinophils, B cells and basophils," explains Ekaterina Gubernatorova, the first author of the article, junior researcher of the Institute of Immunology. "However, in addition to the epithelium, there are more legible sensors of foreign molecules in the lung tissues—macrophages and dendritic cells. By submitting various cytokine signals to their neighbors, they control the strength and quality of the immune response, and interleukin-6 is undoubtedly an important 'word' in the instructions from them."
The scientists proved that interleukin-6 from macrophages helps to form the most common response of T-helper cells of the second type. The main role in this response is played by eosinophil cells, one of the white blood cells, or leukocytes. Interleukin-6, produced by dendritic cells, is involved in more severe asthma subtype, mediated by T-helper cells of the seventeenth type, which are capable of attracting neutrophils into lungs. Neutrophils are the most abundant type of white blood cells, and in severe asthma, they support long-term, non-healing inflammation in the lungs. That is why for such a subtype of the disease so far there is no effective treatment. Thus, interleukin-6 in the future may be a new target for the treatment of asthma, especially for a subtype associated with the neutrophils accumulation in the airways.
More information: Ekaterina O. Gubernatorova et al, Non-redundant Functions of IL-6 Produced by Macrophages and Dendritic Cells in Allergic Airway Inflammation, Frontiers in Immunology (2018). DOI: 10.3389/fimmu.2018.02718