Study finds new pathway for potential glioblastoma treatment

A team led by Texas A&M University's College of Veterinary Medicine & Biomedical Sciences' (CVM) researcher Dr. Stephen Safe has discovered a new pathway that may help suppress the development of glioblastoma tumors, one of the deadliest forms of cancer.
The Texas A&M team's research focuses on the AH receptor, which controls expression of a diverse set of genes, essentially contradicts what was previously understood in glioblastoma research. The Texas A&M study was published in July in the Journal of Biological Chemistry.
"We found the AH receptor—which was previously reported in the literature to be a pro-invasion gene—actually blocked invasion of glioblastoma cells," said Safe, who is a Distinguished Professor of Veterinary Physiology & Pharmacology (VTPP) in the CVM.
"When we add certain AH receptor ligands (molecules that bonds to another molecule), we observed a potent inhibition of glioblastoma cell invasion. Basically, we've shown that it's a good gene that can be targeted by drugs to make it even more effective."
Glioblastomas, the most common and aggressive malignant brain tumor in adults, are comprised of tumor cells that rapidly reproduce and divide, which allow the tumor to grow into nearby normal brain tissue. Currently, these brain tumors are incurable—a patient's median life expectancy after diagnosis is 11-15 months with standard treatments.
According to the American Brain Tumor Association, glioblastomas also form new blood vessels so they can maintain their rapid growth and may use connection fibers to spread to the opposite side of the brain.
Safe said that the tumors are difficult to treat. Because glioblastomas often have finger-like tentacles that spread through the brain, they may not be completely removed through surgery. The tumor's individual cells also respond differently to various therapies.
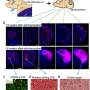
The Texas A&M study used patient glioblastoma cells in collaboration with colleagues at the Detroit Medical Center, as well as cells that were used in previously published glioblastoma studies. The researchers analyzed the AH receptor and several receptor ligands, including Kynurenine.
Previous published studies in the journal Nature found that the AH receptor and Kynurenine were involved in glioblastoma cells' invasion of the brain.
However, the Texas A&M researchers refuted these findings by showing that AH receptors actually serve a protective function and do not promote the invasion of glioblastoma cells. In addition, when researchers added AH receptor ligands but Kynurenine was not active, the level of protection to the brain was enhanced.
These findings suggest that the AH receptor could be a target for the development of drugs to inhibit glioblastoma. The Texas A&M team is now studying the use of the AH receptor as a target for inhibiting glioblastoma and identifying compounds that bind to the AH receptor to provide additional protection to the brain.
"This study opens up a new way for developing potential clinical applications," Safe said. "Whether this line of inquiry will be successful remains to be seen, but our work may offer hope for a disease which has such a poor prognosis."
More information: Un-Ho Jin et al, The aryl hydrocarbon receptor is a tumor suppressor–like gene in glioblastoma, Journal of Biological Chemistry (2019). DOI: 10.1074/jbc.RA119.008882