Oral microbiome contributes to jaw bone health by influencing immune cell interactions with bone cells
It is becoming increasingly clear that the human microbiome—the collection of bacteria, viruses and fungi that live on and within us—significantly contributes to our health. Indeed, several recent studies have demonstrated the contribution of the microbiome to regulating immune cells that influence bone health.
To find out more, researchers at the Medical University of South Carolina (MUSC) who study osteoimmunology, the interface of the skeletal and immune systems, have examined the impact of the oral microbiome on alveolar bone. The alveolar bone, commonly known as the jaw bone, is a unique bone tissue that houses and supports our teeth. Their results, published online on Jan. 25 in the Journal of Clinical Investigation Insight, showed that healthy microbes in the mouth activated a subset of immune cells within the alveolar bone marrow, which in turn promoted osteoclastic cells that are responsible for breaking down bone. They went on to show that depleting the healthy oral microbiome, using an antiseptic mouthwash, protected against this bone loss in preclinical models, demonstrating a direct link between microbes in the mouth and naturally occuring alveolar bone loss.
"The alveolar bone is different from other bone tissues due to its role in supporting the teeth," said Chad M. Novince, D.D.S., Ph.D., associate professor in the colleges of Medicine and Dental Medicine, who studies the impact of the microbiome on osteoimmunology and skeletal metabolism. "What is most fascinating to me is that we were able to show that the commensal oral microbiota modulates the communication between immune cells and bone cells, separate from other microbiota communities, that impact alveolar bone health."
"I think this is really only the start to understanding how the commensal oral microbiome can regulate alveolar bone health and homeostasis," added Jessica D. Hathaway-Schrader, Ph.D., a postdoctoral scholar in the College of Dental Medicine and first author on this study.
Previously, the Novince lab utilized mouse models with a defined microbiota and showed that specific commensal microbes in the gut could influence normal skeletal development and homeostasis. In the current study, they focused on the oral cavity—a unique space in which the microbes colonizing the mouth are in close proximity to the underlying alveolar bone. Little was known about how interactions between microbes and immune cells in the oral cavity, compared with other anatomic sites, influence alveolar bone health.
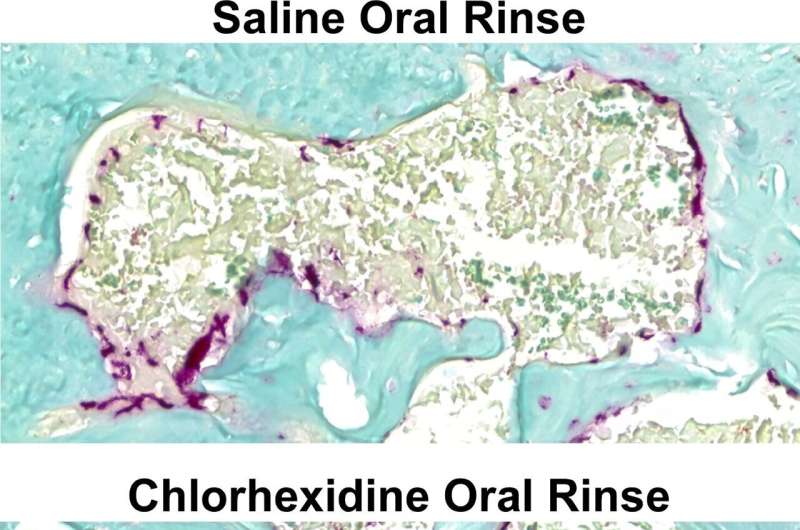
In order to understand the interplay between microbes and immune cells within the oral cavity more fully, the Novince lab pioneered two new techniques. The first technique involved innovatively collecting bone marrow from the mandible of mice, which enabled the researchers to perform in-depth studies on immune cells within alveolar bone. The second technique involved developing a novel way to deplete microbes from the oral cavity of mice. The team utilized a unique delivery sponge loaded with chlorhexidine, an antiseptic used to treat gingivitis, to perform oral rinses on the mice.
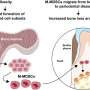
With these innovations in hand, the team used the chlorohexidine rinse to deplete the commensal oral microbiota. Suppressing the commensal microbial load in the oral cavity, while not altering the commensal microbiota at other sites, dampened the immune response in the alveolar bone marrow. This dampened immune response suppressed bone resorbing osteoclast cells, which had an overall protective effect on alveolar bone loss that naturally occurs due to the burden of commensal microbes.
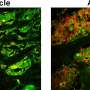
Analysis of the bone marrow within the mandibles of mice revealed that a subset of immune cells were activated by the presence of commensal oral microbes. One important class of activated immune cells were dendritic cells. These cells act like sentinals of the immune system and alert other immune cells that microbial invaders are present. The other important immune cells that were activated by the presence of commensal oral microbes were CD4+ helper T-cells. These cells help to coordinate the immune response during an infection. Ultimately, these immune cells supported osteoclasts.
Together, these data suggest a tightly coordinated pathway in which commensal oral microbes influence alveolar bone health. Furthermore, reducing the burden of commensal microbes in the mouth through oral antiseptic rinses prevented alveolar bone loss, which could have important clinical implications moving forward.
"We were able to show that the commensal oral microbiota influences alveolar bone homeostasis through osteoimmune mechanisms that are distinct from the systemic microbiome," said Novince. "If we are able to suppress the healthy oral microbiome to lower levels, it could help protect from alveolar bone loss, even in a state of health."
This report is the first investigation showing that chlorhexidine reduces naturally occurring alveolar bone loss and suggests that antiseptic oral rinses could support alveolar bone health and homeostasis. To ensure that this potential treatment is safe and effective, future studies aimed at better describing the interaction between the microbiome, immune cells and bone is warranted.
"Although we're broadly suppressing oral microorganisms with the antiseptic rinse, it will be important to determine which specific microbes are really driving this naturally occurring alveolar bone loss," said Hathaway-Schrader. "The alveolar bone marrow is a unique environment, and this is the first step in understanding interactions between oral microbes and immune cells important for promoting bone health."
More information: Jessica D. Hathaway-Schrader et al, Commensal oral microbiota induces osteoimmunomodulatory effects separate from systemic microbiome in mice, JCI Insight (2022). DOI: 10.1172/jci.insight.140738