Investigational drug improves sleep disorder among the blind
An investigational new drug significantly improved a common and debilitating circadian rhythm sleep disorder that frequently affects people who are completely blind, a multicenter study finds. The results were presented Monday at The Endocrine Society's Annual Meeting in San Francisco.
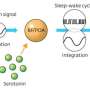
The new drug, called tasimelteon, selectively targets the master body clock in the brain, which controls the timing of the sleep-wake cycle, alertness patterns and the timing of some hormones, as well as many other aspects of physiology and metabolism. This study found that patients who received tasimelteon had a significantly higher rate of re-synchronization of the body clock as compared to patients who received a placebo. The re-synchronization, in turn, led to an increase in night-time sleep, a reduction in day-time sleep, and greater improvement in overall symptoms as rated by the patients' clinicians. During the course of the study, tasimelteon was safe and well-tolerated.
The timing of wakefulness and sleep is controlled by the circadian, or 24-hour, clock in the brain, which is synchronized, or 'entrained' to the 24-hour day by the light-dark cycle. In addition to promoting wakefulness during daylight hours and sleep during the night-time, the circadian clock helps regulate mood, hormonal rhythms and metabolism.
Among people who are completely blind, however, entrainment of the clock is disrupted due to the total lack of light reaching the brain through the eyes. In the absence of light information, the internal clock reverts to its own non-24-hour rhythm, causing a mismatch between rhythms controlled by the clock, such as the sleep-wake cycle, and the 24-hour social world. On average, the internal clock time is approximately 24.5 hours among totally blind people, and while going to sleep half an hour later each day may not sound significant, it does not take long to become completely misaligned from the 24-hour day. In some cases, this disruption is diagnosed as Non-24 Hour Sleep-Wake Disorder, or N24HSWD. Although changes in sleep are most often recognized and addressed by patients, many aspects of well-being are affected because the circadian clock helps regulate so many systems. In addition to interfering with night-time sleep patterns, misalignment of the circadian clock causes daytime drowsiness, which can make it difficult to function socially and professionally.
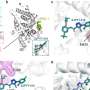
"Tasimelteon addresses the root cause of this disorder by resetting the circadian clock in the brain," said the study's lead author Steven W. Lockley, Ph.D., a neuroscientist at Brigham and Women's Hospital and associate professor at Harvard Medical School in Boston, MA. "The medication is able to replace the time cue usually provided by light and synchronize the circadian clock in totally blind people. None of the traditional medications used to treat sleep disorders or sleepiness have this ability and therefore tasimelteon has the potential to be the first circadian regulator approved by the Food and Drug Administration for the treatment of Non-24 Hour Sleep-Wake Disorder in the blind."
Study participants included 84 patients from 34 medical centers in the United States and Germany. They were between the ages of 18 and 75 years, and 40 percent were female. All participants exhibited disordered sleeping patterns related to total blindness.
Investigators randomly assigned participants to receive either the study drug or a placebo at the same time each day, one hour before their normal bedtime, for the duration of the 26-week study. The study was double-masked, which means that neither investigators nor participants knew which group was receiving tasimelteon.
The effect of the drug on the timing of body clock was assessed from the rhythms of melatonin and cortisol measured in urine samples, in addition to obtaining information about sleep patterns and feelings of well-being.
The study was supported by Vanda Pharmaceuticals, which received Food and Drug Administration approval to study tasimelteon.