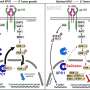
Photodynamic therapy against cancer
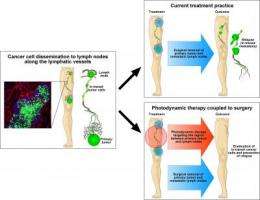
In a new study, published in Science Translational Medicine, researchers at the University of Helsinki, Finland, investigated whether eradicating tumor-associated lymphatic vessels and the tumor cells they contain using photodynamic therapy could reduce tumor metastasis. The results were promising. Previously, the cells in metastatic transit in tumor-draining lymphatic vessels have not been given much attention; so the findings are new and exciting.
Tumor cells have several routes that enable them to move from the primary tumor to distant tissues, a process called metastasis. It is metastasis of the primary tumor that kills most cancer patients. One of the least studied routes of metastasis is the lymphatic system. Many tumors produce factors that promote the formation of new lymphatic vessels (lymphangiogenesis). The newly formed lymphatic vessels enable tumor cells to travel from the primary tumor to the regional lymph nodes from whence they can spread throughout the body.
Current treatment practice is to surgically remove the primary tumor as well as the metastatic lymph nodes, but tumor cells in metastatic transit inside the lymphatic vessels had not been given much attention.
In a new study, Dr Tuomas Tammela and colleagues at the University of Helsinki, Finland, investigated whether eradicating tumor-associated lymphatic vessels and the tumor cells they contain using photodynamic therapy (PDT) with a light-activated cytotoxic drug could reduce or eliminate tumor metastasis. They selected the mouse ear as their model system because it is easy to image both the lymphatic vessels and the in-transit tumor cells.
The researchers implanted mouse melanoma cells or human lung tumor cells into the mouse ear tip and waited two weeks for the primary tumors to become established and to induce lymphangiogenesis. Using deep-tissue microscopy, they observed that the newly formed lymphatic vessels contained in-transit tumor cells as well as small tumor nodules. Using pathology sections taken from a patient with recurrent melanoma, they confirmed that the tumor-associated lymphatic vessels of cancer patients contain in-transit tumor cells and tumor nodules.
However, could PDT eliminate both tumor-associated lymphatic vessels and the tumor cells inside them? The researchers injected verteporfin in a liposomal preparation intradermally into the mouse ear and showed that this cytotoxic dye accumulated specifically in the lymphatic vessels. When they illuminated the mouse ear with infrared laser light, the lymphatic vessels started to shrink and fragment, and became leaky. Also, the researchers found that the mice receiving PDT and surgery had a much lower relapse rate than those that underwent surgery alone.
Using a pig model, the researchers also showed that PDT can target lymphatic vessels deep within the body and, thus, PDT could be useful eradicating tumor-associated lymphatic vessels deep within the tissues of human cancer patients.
"These findings are new and exciting, because the cells in metastatic transit in tumor-draining lymphatic vessels have not been given much attention previously", Dr. Tammela says.
"We do not expect PDT to replace current surgical techniques, which comprise removal of the primary tumor and metastatic lymph nodes. However, PDT could easily be combined with existing surgical techniques to destroy the lymphatic vessels draining from the tumor, as well as the tumor cell aggregates residing within them."
PDT using verteporfin is currently used clinically to destroy overgrown blood vessels in the retina of patients with macular degeneration. As both the drug and the PDT concept are already in use in patients, they are more likely to receive regulatory approval for targeting tumor-associated lymphatic vessels in cancer patients undergoing surgery than drugs still in earlier phases of development, Tammela states.