Asthma vaccine discovery
With asthma now affecting up to one in four New Zealand children, the researchers say this is a promising step in the challenge to understand and control asthma.
The experimental approach is one of the newest frontiers in the rapidly advancing field of immunotherapy, which harnesses the body's own ability to fight diseases.
The research is an extension of work at the Malaghan Institute of Medical Research developing vaccines for cancer by Associate Professor Ian Hermans, in collaboration with synthetic chemist Dr Gavin Painter from the Ferrier Research Institute at Victoria University of Wellington where the vaccines are designed and synthesized.
"Cancer and asthma both involve the immune system, but in cancer we are trying to get the body to take notice of tumour proteins, while in asthma, we want to stop it over-reacting to an allergen," says Dr Hermans.
"Allergy is the wrong sort of immune response. Using the vaccine, we have initiated a more appropriate immune response and prevented the allergy from taking hold."
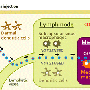
Vaccines work by presenting the body with an antigen, which provokes an immune response. This involves activating T cells, produced by the body's immune system, which are then ready to protect from the disease in the future.
To strengthen the immune response, a chemical called an adjuvant is administered along with the antigen, to make the vaccine more effective.
In the asthma vaccine, the antigen and the adjuvant are chemically linked, rather than simply co-delivered. This novel approach ensures the essential components reached the target cells together and created the most powerful but highly specific immune response that targets the disease.
Dr Herman's says preparing the linked vaccine required some "pretty clever chemistry".
"By linking them, we make sure they are both delivered to the right place in the body. Once there, they are split and presented to the immune system to initiate a response," he says.
The idea of using a vaccine to prevent asthma was the brainchild of Malaghan Institute Professor Franca Ronchese who explains how the vaccine works.
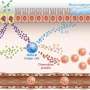
"In asthma, allergens such as those produced by house dust mites are inhaled and taken up by dendritic cells in airways, causing inflammation and many of the symptoms of asthmatic disease. With the vaccine, we think we can direct other immune cells, the killer T-cells, to go and block the dendritic cells, so they stop sending out the wrong messages. It's like taking out the generals of the enemy's army in order to overpower it," she says.
The linked vaccine technology could in principle be applied to other allergic diseases. Patent protection has been obtained and opportunities to commercialise the technology are currently being pursued.