Stem cell-based therapy for targeting skin-to-brain cancer
Investigators from Brigham and Women's Hospital (BWH) and the Harvard Stem Cell Institute have a potential solution for how to kill tumor cells that have metastasized to the brain. The team has developed cancer-killing viruses that can deliver stem cells via the carotid artery, and applied them to metastatic tumors in the brain of clinically relevant mouse models. The investigators report the elimination of metastatic skin cancer cells from the brain of these preclinical models, resulting in prolonged survival. The study, published online this week in the journal PNAS, also describes a strategy of combining this therapy with immune check point inhibitors.
"Metastatic brain tumors - often from lung, breast or skin cancers - are the most commonly observed tumors within the brain and account for about 40 percent of advanced melanoma metastases. Current therapeutic options for such patients are limited, particularly when there are many metastases," says Khalid Shah, MS, PhD, director of the Center for Stem Cell Therapeutics and Imaging (CSTI) in the BWH Department of Neurosurgery, who led the study. "Our results are the first to provide insight into ways of targeting multiple brain metastatic deposits with stem-cell-loaded oncolytic viruses that specifically kill dividing tumor cells."
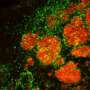
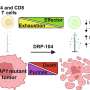
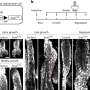
In their search for novel, tumor-specific therapies that could target multiple brain metastases without damaging adjacent tissues, the research team first developed different BRAF wild type and mutant mouse models that more closely mimic what is seen in patients. They found that injecting patient-derived, brain-seeking melanoma cells into the carotid artery of these preclinical models resulted in the formation of many metastatic tumors throughout the brain, mimicking what is seen in advanced melanoma cancer patients. The injected cells express markers that allow them to enter the brain and are labelled with bioluminescent and fluorescent markers to enable tracking by imaging technologies.
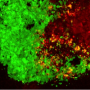
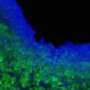
To devise a potential new therapy, the investigators engineered a population of bone marrow derived mesenchymal stem cells loaded with oncolytic herpes simplex virus (oHSV), which specifically kills dividing cancer cells while sparing normal cells. Previous research by Shah and his colleagues shows that different stem cell types are naturally attracted toward tumors in the brain. After first verifying that stem cells injected to the brain would travel to multiple metastatic sites and not to tumor-free areas in their model, the team injected stem cells loaded with oHSV into the carotid artery of metastasis-bearing mice.. Injecting the stem cells loaded with oHSV into the carotid artery, a likely strategy for clinical application, led to significantly slower tumor growth and increased survival, compared with the models that received unaltered stem cells or control injections. The oHSV loaded stem cells are ultimately killed by oHSV mediated oncolysis, preventing the engineered cells from persisting within the brain, which is an important safety component in the therapeutic use of these stem cells.
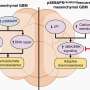
Due to an increasing body of evidence which suggests that the host immune response may be critical to the efficacy of oncolytic virotherapy, Shah and his colleagues also developed an immunocompetent melanoma mouse model and explored treating with both stem cell loaded oHSV and immune checkpoint blockers such as the ones that target the PD-1/PD-L1 pathway. They found that PD-L1 immune checkpoint blockade significantly improved the therapeutic efficacy of stem cell based oncolytic virotherapy in melanoma brain metastasis.
"We are currently developing similar animal models of brain metastasis from other cancer types as well as new oncolytic viruses that have the ability to specifically kill a wide variety of resistant tumor cells," said Shah, who is also a professor at Harvard Medical School and a principal faculty member at the Harvard Stem Cell Institute. "We are hopeful that our findings will overcome problems associated with current clinical procedures. This work will have direct implications for designing clinical trials using oncolytic viruses for metastatic tumors in the brain."
More information: Wanlu Du el al., "In vivo imaging of the fate and therapeutic efficacy of stem cell-loaded oncolytic herpes simplex virus in advanced melanoma," PNAS (2017). www.pnas.org/cgi/doi/10.1073/pnas.1700363114